2013 Volume 2 - Issue 1
-
November 19, 2013 Research Article
 Abstract Introduction: An elevated level of plasma homocysteine (eHcy) is a recognized risk factor for many neurological conditions. Recent laboratory studies show a toxic effect of homocysteine causing neuropathy. Clinical observations disclosed that eHcy ex.....
Abstract Introduction: An elevated level of plasma homocysteine (eHcy) is a recognized risk factor for many neurological conditions. Recent laboratory studies show a toxic effect of homocysteine causing neuropathy. Clinical observations disclosed that eHcy ex..... -
November 19, 2013 Mini Review
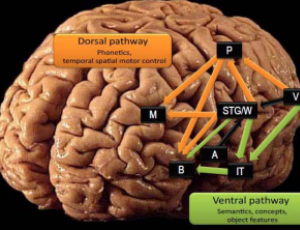 Abstract Aphasia and apraxia are two major neuropsychological syndromes that in most cases are caused by injuries in the left cerebral hemisphere. Clinical studies have revealed a double dissociation between aphasia and apraxia, and a strong correlation in th.....
Abstract Aphasia and apraxia are two major neuropsychological syndromes that in most cases are caused by injuries in the left cerebral hemisphere. Clinical studies have revealed a double dissociation between aphasia and apraxia, and a strong correlation in th..... -
November 19, 2013 Research Article
 Abstract Objective: The purpose of this study is to achieve beneficial treatment outcomes for severe intractable epilepsy patients using neurophysiologically guided stereotactic multitarget surgery. Material and methods: Ninety-three patients (64 men, mean .....
Abstract Objective: The purpose of this study is to achieve beneficial treatment outcomes for severe intractable epilepsy patients using neurophysiologically guided stereotactic multitarget surgery. Material and methods: Ninety-three patients (64 men, mean ..... -
November 20, 2013 Research Article
 Abstract Background: High blood pressure (BP) in an acute stroke has been demonstrated to result in a poor prognosis in several studies; however, controversial results were obtained. This study was designed to investigate the correlation between an initial hi.....
Abstract Background: High blood pressure (BP) in an acute stroke has been demonstrated to result in a poor prognosis in several studies; however, controversial results were obtained. This study was designed to investigate the correlation between an initial hi..... -
December 16, 2013 Research Article
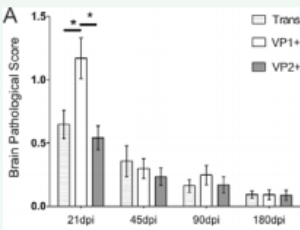 Abstract We used transgenic expression of capsid antigens to Theiler’s murine encephalomyelitis virus (TMEV) to study how the immune response to VP1 and VP2 influences spinal cord demyelination, remyelination and axonal loss during the acute and chronic pha.....
Abstract We used transgenic expression of capsid antigens to Theiler’s murine encephalomyelitis virus (TMEV) to study how the immune response to VP1 and VP2 influences spinal cord demyelination, remyelination and axonal loss during the acute and chronic pha..... -
November 20, 2013 Research Article
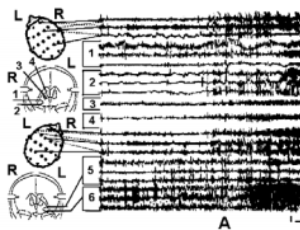 Abstract Objective: The purpose of this study is to achieve beneficial treatment outcomes for severe intractable epilepsy patients using neurophysiologically guided stereotactic multitarget surgery. Material and methods: Ninety-three patients (64 men, mean a.....
Abstract Objective: The purpose of this study is to achieve beneficial treatment outcomes for severe intractable epilepsy patients using neurophysiologically guided stereotactic multitarget surgery. Material and methods: Ninety-three patients (64 men, mean a.....