Journal of Substance Abuse and Alcoholism
Volume 5 - Issue 4 Articles
-
ArticleDecember 14, 2017 | Pages : 205 - 450Abstract Background: Alcohol withdrawal and benzodiazepine withdrawal present in similar fashions, but can be difficult to differentiate with a muddled history of polysubstance use and psychiatric disorders especially in acute settings. Case presentation: W.....
-
ArticleNovember 18, 2017 | Pages : 205 - 450Abstract While smoking prevalence is showing a decline in high income countries (HIC), smoking among pregnant women has also reduced and current prevalence in certain HIC is between 8.4 to 11.4%. In low and middle-income countries (LMIC), exposure to second.....
-
ArticleNovember 08, 2017 | Pages : 205 - 450Abstract The real trouble with mass casualty events is that they are thought of as events. As if there is some beginning, middle and end that play out in a logical sequence with tidy openings and closures. Little Romeo and Juliets that fragment tragedy, makin.....
-
ArticleSeptember 07, 2017 | Pages : 205 - 450Abstract Introduction: Drug abuse places a heavy burden on public health systems in terms of treatment, care, prevention and their health consequences.The objective of this study was to determine risk factors associated with drug abuse among Malay males FELDA.....
Volume 5 - Issue 3 Articles
-
ArticleJuly 21, 2017 | Pages : 205 - 450Abstract Initially created in the 1950’s as an anesthetic, 1-phenylcyclohexylpiperidine or PCP as it commonly called, has become a problem for the youth of today. This highly volatile chemical is synthesized in underground laboratories throughout the United.....
-
ArticleJune 23, 2017 | Pages : 205 - 450Abstract Mental and substance use disorders are the leading cause of disability and associated burden globally and in Sub-Saharan Africa. Major mental disorder has the largest burden, yet the very limited mental health treatments in Sub-Saharan Africa are fre.....
-
ArticleMay 31, 2017 | Pages : 205 - 450Abstract The World Health Organization (WHO) recently estimated that approximately 2.3 million individuals worldwide are coinfected with Human Immunodeficiency Virus (HIV) and Hepatitis C Virus (HCV). HIV-infected individuals were, on average, 6 times more li.....
-
ArticleMay 24, 2017 | Pages : 205 - 450Abstract Powdered alcohol or “palcohol” was originated in the 1970s, but resurfaced in 2007 in the Netherlands and again in the United States in 2014. The concept for powdered alcohol is that it can be sold cheaply in small packets and mixed with water. O.....
-
ArticleApril 27, 2017 | Pages : 205 - 450Abstract Most individuals have daily, if not constant access to the internet. The increased accessibility of internet use has coincided with an increased availability and social acceptance of gambling behaviours. This trend increases the possibility that gamb.....
Volume 5 - Issue 2 Articles
-
ArticleCarmen Fernández Caceres José Luis Alba Robles Solveig Eréndira Rodríguez Kuri Valeriano Raúl García AurrecoecheaApril 14, 2017 | Pages : 205 - 450Abstract This article presents the first Mexican study about the relationship between cocaine/crack use disorder and antisocial behavior, based on the comparison of cocaine/crack patients and non stimulant drug patients (attended for alcohol, cannabis, heroin.....
-
ArticleAnujh Maharajh Christian Smith Daena-Camille Ballack Fadilah Khan Kameel Mungrue Nikolai Lewis Racheal LeoApril 24, 2017 | Pages : 205 - 450Abstract Background: Alcohol consumption is a major contributor to morbidity and mortality and hence is an important and ongoing public health challenge. While alcohol abuse and dependence have historically received the greatest attention, the detection and t.....
-
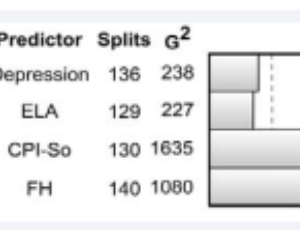
ArticleApril 19, 2017 | Pages : 205 - 450Abstract Objective: A family history (FH+) of alcoholism or other substance use disorders (SUD) is an SUD risk factor in the offspring, although not all FH+ develop an SUD. To explore SUD predictors, we examined the joint impact of antisocial characteristics .....

-
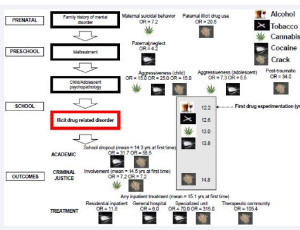
ArticleCamila Da Silva Barbosa Camila Ribas Stefanello Stephan Espinosa Meirelles Emile Hirdes Kruger Maicon Bonaldo DiasFebruary 14, 2017 | Pages : 205 - 450Abstract Most of the available information about risk factors for specific illicit drug related disorders (cannabis, cocaine powder and crack cocaine) during adolescence comes from studies that analyze the use of illegal substances as a single group. This stu.....
-
ArticleMarch 25, 2017 | Pages : 205 - 450Abstract The aim of the study was to explore the substance abuse/drug use related knowledge and attitudes among youth in Addis Ababa, Ethiopia. Substance abuse and dependence are one of the most frequently occurring disorders in adolescents, young adults, and.....
Volume 5 - Issue 1 Articles
-
ArticleSamh Pratt Amy Harrington Daniel Colctti Delbert Robinson Gregory C. MoHugo Haiyi Xie Jill Williams Joelle C. Feiron Kelly Aschbrenner Mary Ann Greene Mary F. Brunette Timothy DevittMarch 23, 2017 | Pages : 205 - 450Abstract Background: Over half of young adults with schizophrenia smoke. Quitting before age 30 could prevent some of the disparate morbidity and mortality due to smoking-related diseases. However, little research has addressed smoking in this group nor evalu.....
-
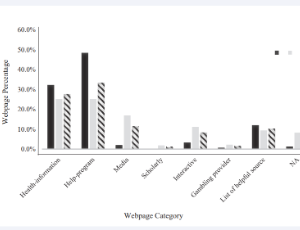
ArticleMarch 10, 2017 | Pages : 205 - 450Abstract Though male sex work is a global phenomenon, systematic reviews on this topic are scant. Our understanding of scholars’ perspectives on this topic remains unclear. The article reviews past and recent social science research on male sex work. First,.....
-
ArticleFebruary 08, 2017 | Pages : 205 - 450Abstract Meditation/mindfulness based approaches offer a wealth of new ways to assess and intervene with those struggling with the challenges of substance use disorders. In this paper, I will introduce some of the core concepts and languages of a meditation/m.....
-
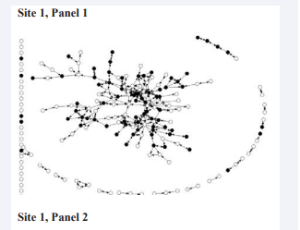
ArticleAmanda Yoshioka-Maxwell Anamika Barman Adhikari Eric Rice Hailey Winetrobe Harmony Rhoades Robin PeteringJanuary 19, 2017 | Pages : 205 - 450Abstract Homeless youth report more marijuana use than stably housed youth; their marijuana use has been linked to the marijuana-using behaviors of their peers. This study was the first to examine the process of network influences in marijuana use with popula.....
-
ArticleJanuary 03, 2017 | Pages : 205 - 450Abstract Study objective: To characterize national hospital practices for treating patients with ethanol for alcohol withdrawal syndrome. Design: Cross-sectional survey Setting: A 9-item survey conducted via telephone or email. Participants: Physician, cl.....
Browse by Year
Author Information
X
Subscribe to Newsletters
And stay informed about our news and events