Evaluation of Diagnostic Methods for Births Related Clavicle Fractures of Newborn
- 1. Meltem Karabay1*
ABSTRACT
Objectives: The aim of this study is to investigate the role of ultrasonography (US) and physical examination findings in the diagnosis of NCF in traumatic births.
Methods: This study was done between July 1st, 2019 and March 31st, 2020. Physical examination, X-ray and US were performed to detect the presence of fracture in traumatic newborns. All newborns were monitored using US by the same radiologist. The obtained data were analyzed statistically by software (SPSS) .
Results: A total 59/88 (67.0%), fractures were detected and 1/6 (16.7%), of the traumatized newborns delivered by cesarean, whereas 58/82 (70.7%), of the traumatized newborns born via vaginal delivery (p = 0.014). The diagnostic specificity value of US alone was found as 96.6% diagnostic sensitivity of US alone was 79.7%, it increased up to 98.3% in combinations where crepitation exists, yet Moro reflex is absent. A value of 100%, which is the highest specificity, was reached when the US and the presence of crepitation were evaluated together.
Conclusions: This study demonstrated that NCF is accurately diagnosed using US rather than plain X-ray. In a detailed examination carried out using US, the presence of crepitation, indication of a slight pain and the absence of the Moro reflex are significant to represent the NCF. If suspicious findings are obtained with physical examination, US is sufficient for diagnosis.
KEYWORDS
• Clavicle; Fractures; Newborn; Birth; Ultrasonography
CITATION
Karabay M, Yümnü Y, Altunsoy D, Ekerbiçer HÇ, Caner ?. Ann Pediatr Child Health 2021; 9(1): 1223.
ABBREVIATIONS
CS: Cesarean Section; LR: Likelihood Ratio; NCF: Newborn Clavicle Fracture; NPV: Negative Predictive Value;PPV: Positive Predictive Value; SPSS: Statistical Package For The Social Sciences; US: Ultrasonography; VD : Vaginal Delivery
INTRODUCTION
Newborn clavicle fracture (NCF), is the most common newborn fracture with 0.4-2% frequency [1]. NCF is usually unilateral and often associated with manipulation of the arm and shoulder during labor. Even though it is mostly observed in vaginal delivery (VD), it might occur following cesarean section (CS), as well [2]. NCF is most routinely diagnosed with reduced arm motion and palpation on a careful examination. The examination findings reveal that most of these newborns exhibit minimum or no symptoms in the first few days [3]. Therefore, identifying a clavicle fracture is difficult in the first days of life.
NCF mostly represents green tree fracture type. Following the diagnosis of the fracture on a newborn, movement of the arm, which is located on the fracture side, is hindered by simple methods. In case of missing the fracture diagnosis, usually no complications occur. However, the swelling that occurs during recovery might alert parents [4]. Swelling caused by callus tissue, which occurs when bones unite, becomes visible since the fracture line is found under the skin. Informing the relatives of this situation beforehand will prevent their agitation [5].
Imaging techniques such as X-ray are significant to confirm the diagnosis of NCF. However, radiography is time consuming, costly and exposes patients to undesirable effects. Yet, according to the ALARA principle, even the least dose of radiation might cause chromosomal mutations along with stochastic effects and initiate the malign process [6,7]. Similarly, ALARA radiation safety principles are harmful at all levels of ionizing radiation [8,9]. It is important to diagnose newborns with more innocent methods other than radiation for NCF diagnosis [10]. The presence of crepitation in the physical examination of the NCF or the arm movements of the newborn and related reflexes are of great importance. However, the diagnostic value of physical examination findings is not clearly defined. In this study, we aimed to investigate the characteristics and related factors of NCF and evaluate the diagnostic accuracy of certain examination findings and diagnostic methods that could be alternative to X-ray, such as ultrasonography (US).
MATERIALS AND METHODS
XXXXXXX provinence, located in the eastern XXXXXX region of Turkey. XXXXXXX Training and Research Hospital has a bed capacity of 1100, consists of three different campuses and serves approximately one million people. This research was conducted in the women’s and children’s hospital campus. An average of 15- 20 deliveries are made every day in this hospital.
This research is a prospective evaluation study of US testing compared to a reference standard clavicle X-ray test. This study was planned as descriptive, cross-sectional which include all traumatic deliveries followed up in our hospital between July 1st, 2019 and March 31st, 2020.
Newborns delivered traumatically in our hospital during the study period were included in the study. All study patients were examined by a neonatologist (MK), as soon as possible and traumatic newborns were included in the study after obtaining parental consent. During this examination, crepitation and sensitivity on the clavicle were investigated. The presence of crepitation in a newborn was determined through feeling the crepitation by clavicle area palpitation. Additionally, Moro reflex was examined.
Information regarding the gestational age, birth weight, head circumference, gender, the delivery type (VD, CS, forceps or vacuum assisted VD), were recorded. Only term newborns were included, preterm births were excluded from the study.
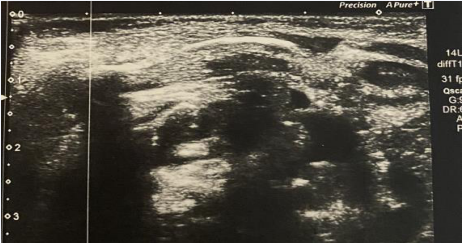
All radiological examinations and radiology reports were made by the radiology expert (YY). Toshiba Aplio 400 device was used for US. US examination was performed on both clavicles. Discontinuity of bone echogenicity was defined as fracture. Mobility of fragments was investigated during respiration. Clavicle fracture was investigated in the image (Figure 1).
Figure 1 Ultrasonography appearance of clavicle fracture.
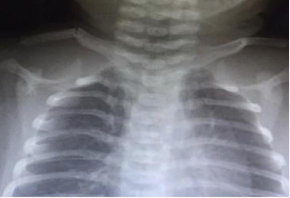
The babies were sent to the hospital’s radiology unit for imaging, which was obtained in suppin position at a dose of 55 KW, 1.60 mAS. Clavicle fracture was investigated in the image (Figure 2).
Figure 2 X-ray appearance of clavicle fracture.
The findings are represented as Mean ± STD along with percentages. Shapiro-Wilk test was used for the normality assumption. Chi-Square test (with Continuity Correction), Fisher’s Exact test, Independent Samples test and Mann-Whitney tests were performed when necessary. Sensitivity, specificity, positive likelihood ratio, negative likelihood ratio, positive predictive value, negative predictive value and accuracy values (with 95% confidence intervals), were calculated to determine the diagnostic validity of some findings that could be alternative to X-ray in diagnosing fractures. During these calculations, the prevalence value was assessed as 67% (59/88). P value less than 0.05 was considered statistically significant. IBM SPSS Statistics version 20.0 (SPSS Inc., Chicago, USA) and MedCalc (Version 19.4.1.) were used for statistical analysis. Ethical approval for this study was obtained from XXXXXX University Faculty of Medicine Ethics Committee. (28/06/2019-E.8499).
RESULTS AND DISCUSSION
During the study period (July, 1 2019 – March, 31 2020), a total of 4124 babies were born in our hospital. Of these deliveries, 2211 (54%), occurred through VD, whereas 1913 (46%), were CS. A total of 92 (92/4124, 2%), traumatic births were detected. However, four patients did not enroll in the study due to not providing informed consent (three patients had excessive family agitation, other one fear of pain, respectively). Some characteristics of the remaining 88 traumatic newborns, mothers and births are presented in the table (Table I).
|
Table 1: Demographical characteristics of the newborns and mothers. |
|
|
Characteristics |
Number |
|
Gestational week (mean ± STD) |
39.1± 1.2 |
|
Birth weight (g) (mean ± STD) |
3478.9 ± 491.3 |
|
Gender (male) |
43 (48.9%) |
|
Height (cm) (mean ± STD) |
50.7±1.4 |
|
Head circumference (cm) (mean ± STD) |
34.8 ± 0.9 |
|
Maternal diabetes |
3 (3.4%) |
|
Maternal obesity |
3 (3.4%) |
|
Cesarean section / Vaginal delivery |
6/82 (6.8%/93.1%) |
|
Use of vacuum or forceps |
4 (4.5%) |
|
Mother’s age (mean ± STD) |
27.3 ± 5.7 |
|
Primiparous |
45 (51.1%) |
|
Parity (mean ± STD) |
1.8 ± 1.0 |
While the probability of traumatic delivery was 82/2211 (3.9%), in VD, this value decreased to 6/1913 (0.10%), in CS (p = 0.0000). The fractures were detected 1/6 (16.7%), of traumatized infants born by CS, whereas 58/82 (70.7%), of the traumatized infants born by VD (p = 0.014).
X-ray and US were used to diagnose fractures in 59 (67%), and 47 (53.4%), of the traumatic births, respectively. Findings related to the birth trauma are summarized in the table (Table 2).
|
Table 2: Distribution of traumatic status in newborns. |
||
|
Traumatic Status (n=88) |
Number (%) |
Explanation |
|
Fractures were diagnosed with X-ray |
59 (67.0) |
40 on right, 19 on left* |
|
Fractures were diagnosed with ultrasonography |
47 (53.4) |
32 on right, 15 on left |
|
Crepitation with physical examination |
57 (64.8) |
38 on right, 19 on left |
|
Absence of the Moro reflex |
8 (9.1) |
6 on right, 2 on left |
In this study, we compared different diagnosis methods with reference methods (X-ray).
The success of the presence of crepitation, which is an examination finding, in detecting fractures were investigated. It found that 3 of 31 (9.7%), babies absence of crepitation and 56 out of 57 (98.2%), babies with crepitation had fractures (p = 0.000).
There was no significant relationship between the presence of fracture and characteristics of birth, baby and mother (Table 3).
|
Table 3: Evaluating the relationship between diagnostic methods and characteristics of the demographical properties. |
|||
|
Characteristics of trauma, newborn and birth |
X-ray diagnosed fracture |
p value |
|
|
Yes |
No |
||
|
Number (%) |
Number (%) |
||
|
Presence of crepitation |
56 (98.2) |
1 (1.8) |
0.000** |
|
Absence of the Moro reflex |
5 (62.5) |
3 (37.5) |
1.000* |
|
Use of vacuum or forceps |
2 (50.0) |
2 (50.0) |
0.596* |
|
|
Mean ± STD |
Mean ± STD |
|
|
Age of the mother |
27.3±6.0 |
27.3±5.1 |
0.990*** |
|
Number of pregnancies |
2.4±1.5 |
2.3±1.6 |
0.901**** |
|
Parity |
1.8±1.1 |
1.7±0.9 |
0.973**** |
|
Gestational week |
39.1±1.2 |
39.3±1.2 |
0.353**** |
|
Birth age (hour) |
3508.4±463.1 |
3418.8±547.8 |
0.619**** |
|
Height (cm) |
50.7±1.4 |
50.7±1.4 |
0.554**** |
|
Head circumference (cm) |
34.8±0.9 |
34.8±0.9 |
0.908**** |
|
* Fisher’s Exact Test was used. ** Chi-Square Test (with Continuity Correction) was used. ***Independent Samples Test was used. ****Mann-Whitney Test was used |
|||
The sensitivity of US alone was 79.7%, whereas this percentage increased to 98.3% when US was evaluated together with the presence of crepitation and the absence of the Moro reflex. The specificity value of US alone was calculated as 96.6%. In the case of evaluating US and the presence of crepitation together, this value has reached up to 100%.
Positive likelihood ratio (LR), could not be calculated in cases where US and crepitation exist together. US alone had the highest positive LR (23.1), while the lowest LR was 5.7 in other combinations. Negative LR values varied between 0.02 and 0.24. Combinations of US and the presence of crepitation together represented the highest negative LR value, whereas combinations with US or the presence of crepitation or the absence of the Moro reflex had the lowest negative LR value. The combination, in which US and crepitation exist and were evaluated together, exhibited the highest positive predictive value (PPV), value (100%). The highest negative predictive values (NPV), has been accomplished (96.4%), when the presence of US or crepitation, in other words the conditions where one of them was positive, has been evaluated as fracture. The comparison X-ray and other methods to diagnosis of clavicle fracture were presented in table (Table 4).
|
Table 4: Comparison of the some diagnostic methods when X-ray is considered as the gold standard. |
|||||
|
US only |
Radiograph |
US and crepitation |
Radiograph |
||
|
Fracture |
No Fracture |
Fracture |
No Fracture |
||
|
Fracture |
47 |
1 |
Fracture |
45 |
0 |
|
No Fracture |
12 |
28 |
No Fracture |
14 |
29 |
|
US or crepitation |
Radiograph |
US or crepitation or the absence of the Moro reflex |
Radiograph |
||
|
Fracture |
No Fracture |
Fracture |
No Fracture |
||
|
Fracture |
58 |
2 |
Fracture |
58 |
5 |
|
No Fracture |
1 |
27 |
No Fracture |
1 |
24 |
|
US: Ultrasonography |
|||||
The diagnostic values of US and other findings are demonstrated in the table (Table 5).
|
Table 5: Evaluation of the validity and reliability of some diagnostic methods to identify the clavicle fracture in babies who exposed to traumatic birth, when X-ray is considered as the gold standard. |
|||||||
|
Diagnostic Method |
Sensitivity (95% CI) |
Specificity (95% CI) |
Positive Likelihood Ratio (95% CI) |
Negative Likelihood Ratio (95% CI) |
Positive Predictive Value (95% CI) |
Negative Predictive Value (95% CI) |
Accuracy (95% CI) |
|
US only |
79.7% (67.2-89.0) |
96.6% (82.2-99.9) |
23.10 (3.35-159.19) |
0.21 (0.13-0.35) |
97.9% (87.2-99.7) |
70.0% (58.4-79.6) |
85.2% (76.1-91.9) |
|
US and |
76.27% |
100.0% |
|
0.24 |
100.0% |
67.5% |
84.1% |
|
crepitation* |
(63.4-86.4) |
(88.1-100.0) |
(0.15-0.37) |
|
(56.8-76.6) |
(74.8-91.0) |
|
|
US or |
98.3% |
93.1% |
14.25 |
0.02 |
96.7% |
96.4% |
96.6% |
|
crepitation ** |
(90.9-99.9) |
(77.2-99.1) |
(3.7-54.3) |
(0.00-0.13) |
(88.4-99.1) |
(79.5-99.5) |
(90.4-99.3) |
|
US or |
|
|
|
|
|
|
|
|
crepitation or the absence of the Moro reflex |
98.3% (90.9-99.9) |
82.8% (64.2-94.2) |
5.70 (2.57-12.7) |
0.02 (0.00-0.14) |
92.1% (83.9-96.3) |
96.0% (77.4-99.4) |
93.2% (85.7-97.5) |
|
*** |
|
|
|
|
|
|
|
|
US: Ultrasonography * Fracture is considered as positive when the presence of fracture in USG and the crepitation are both positive on examination. ** Fracture is considered as positive when either the presence of fracture in USG or the crepitation is positive on examination. *** Fracture is considered as positive when either the presence of fracture in USG or the existence of crepitation or the absence of the Moro reflex is positive on examination. |
|||||||
DISCUSSION
In this study, it found that the probability of having traumatic deliveries following CS was found relatively lower, whereas this rate was much higher in VD. The probability of birth trauma was determined as 2.1% (88/4124), in our center. Similarly, previous studies have demonstrated that birth traumas in Turkey were between 0.7-2.2% [11]. The rate stated in our research includes all live births during the study period. Our hospital is a tertiary health center, where emergency births are directed to our center. Therefore, our rate of birth trauma is at close proximity to the upper limit of our country.
NCF are usually associated with the mode of delivery [12]. NCF is extensively common in birth-related traumas [13]. These fractures usually do not cause disability or deformity in the baby [1,14]. NCF risk is low in CS, yet it increased significantly in VD. In this study, NCF was detected in 70.7% of traumatic VD and only 16.7% of traumatic CS (p=0.0065). Specifically, NCF is more frequent in deliveries with abnormal presentation of the baby[15]. The widest part of a baby’s body in the womb is the shoulders. This area handles the main burden of the baby during birth. Using forceps or vacuum to move the baby forward during a difficult birth and the manipulations that include applying pressure to the uterus usually cause collarbone breaks, which is a thin and fragile tubular bone. We would like to mention that the reason for not having any breech position in our study is highly related with preferring CS in breech presentations.
Radiography has been applied in NCF diagnosis for many years. Diagnosis of a NCF can be verified using X-ray. However, this method exposes babies to radiation and significant time and resources consuming. US is cheaper, more harmless and more environmentally friendly than X-ray. US can show the weak bones of the newborn better than an x-ray. Moreover, it causes less damage since it does not contain ionizing radiation. According to our findings, US is a reliable alternative for the diagnosis of NCF. More importantly it does not expose the patient with radiation, thus it is not carcinogenic. However, US requires experienced personnel.
US has been used for years to diagnose NCF [16]. However, the first time with this study that physical examination findings towards NCF, along with US, were compared with X-ray. According to the findings we obtained in this study, we observed that physical examination still has a very valuable place in defining NCF despite the developing technology. We also found that some examination findings (such as presence of crepitation, absence of Moro reflex), correspond to sufficient sensitivity and specificity to define NCF. It found that crepitation sense during the clavicle examination of newborn has a very effective diagnostic value in detecting NCF. Crepitation on the clavicle may be investigated after birth for the diagnosis of NCF. Also, examining the presence of crepitation after a traumatic delivery is very important for the diagnosis of NFC.
According to our findings, even in countries with limited resources and limited access to US, fracture is confirmed when crepitation is detected during the examination after a birth trauma.
However, not all babies with NCF show crepitation during physical examination. US may be considered for such situations.
Approximately 40% of NCF’s heal without ever being identified. However, if a fracture is detected later by the family, it may cause legal problems [17]. Such fractures can be easily detected in the hospital with an US at the bedside and a careful examination.
The most common Clavicle fracture associated symptom is arm movement related pain and agitation. The affected arm is usually not mobile like the intact arm. In case of a damage in arm nerves, the baby will face difficulty in moving arms or the arm will hang down on its side. All these findings should be carefully examined by a clinician. Also, there is a risk of unnoticing NCF if the examination is not performed carefully. It should be remembered that sometimes NCF is not associated with any signs or symptoms. Therefore, it is not easy to diagnose [18]. It is usually detected within 7 to 10 days after birth and when a callus appears [7]. This is the reason behind diagnosing NCFs after discharge. Sometimes, discoloration is observed in the fracture area. Passive movement of the arm yields screams of pain. Palpation reveals tenderness, crepitation, and irregularity throughout the clavicle [1].
Evaluation of US and examination findings together is significantly crucial. According to our findings, the possibility of NCF can be excluded in deliveries without crepitation and with negative US result and X-ray monitoring is not required for such a baby.
CONCLUSION
This study demonstrates that US accurately diagnoses clavicle fractures compared to plain radiographs. Reporting the existence of pain and crepitation confirmed by the US and a detailed examination is more significant than conforming the absence of the Moro reflex when it comes to diagnosing NCF. In traumatic newborns, a good extremity examination should be performed first, and if the obtained findings are compatible with NCF, diagnostic confirmation using the US will be sufficient.
REFERENCES
- Beall MH, Ross MG. Clavicle fracture in labor: risk factors and associated morbidities. J Perinatol. 2001; 21: 513-515.
- Kanik A, Sutcuoglu S, Aydinlioglu H, Erdemir A, Arun Ozer E. Bilateral clavicle fracture in two newborn infants. Iran J Pediatr. 2011; 21: 553- 555.
- Hsu TY, Hung FC, Lu YJ, Ou CY, Roan CJ, Kung FT, et al. Neonatal clavicular fracture: clinical analysis of incidence, predisposing factors, diagnosis, and outcome. Am J Perinatol. 2002; 19: 17-21.
- Reiners CH, Souid AK, Oliphant M, Newman N. Palpable spongy mass over the clavicle, an underutilized sign of clavicular fracture in the newborn. Clin Pediatr. 2000; 39: 695-698.
- Shannon EG, Hart ES, Grottkau BE. Clavicle fractures in children: the essentials. Orthop Nurs. 2009; 28: 210-214.
- Joseph PR. Clavicular Fractures in Neonates: Frequency vs Significance-Reply [Internet]. Arch Pediatric Adolescent Med. 1991;145: 251.
- Joseph PR. Clavicular Fractures in Neonates [Internet]. Arch Pediatr Adolesc Med. 1990;144: 165.
- Halm BM, Chaudoin LT. Diagnosis of a Posterior Fracture Dislocation of the Medial Clavicle in an Adolescent With Point-of-Care Ultrasound. Pediatr Emerg Care. 2017; 33: 519-521.
- Cross KP, Warkentine FH, Kim IK, Gracely E, Paul RI. Bedside Ultrasound Diagnosis of Clavicle Fractures in the Pediatric Emergency Department. Academic Emerg Med. 2010; 17: 687-693.
- South M, Isaacs D. Practical Paediatrics E-Book: With STUDENT CONSULT Online Access. Elsevier Health Sciences. 2012.
- Çolak R, Çoban K, Çelik K, Ergon EY, Özdemir SA, Olukman Ö, et al. Birth Injuries: Assessment Of Clinical Findings And Maternal, Fetal And Obstetric Risk Factors. J Behcet Uz Children s Hospital. 2017.
- Sananès N. Breech Presentation: CNGOF Guidelines for Clinical Practice - Benefits and Risks for the Neonate and Child of Planned Vaginal Delivery versus Elective Cesarean Section. Gynecol Obstet Fertil Senol. 2020; 48: 95-108.
- Roberts SW, Hernandez C, Maberry MC, Adams MD, Leveno KJ, Wendel GD Jr. Obstetric clavicular fracture: the enigma of normal birth. Obstet Gynecol. 1995; 86: 978-981.
- Rehm A, Promod P, Ogilvy-Stuart A. Neonatal birth fractures: a retrospective tertiary maternity hospital review. J Obstet Gynaecol. 2020; 40: 485-490.
- Katz R, Landman J, Dulitzky F, Bar-Ziv J. Fracture of the clavicle in the newborn. An ultrasound diagnosis. J Ultrasound Med. 1988; 7: 21-23.
- Kayser R, Mahlfeld K, Heyde C, Grasshoff H. Ultrasonographic imaging of fractures of the clavicle in newborn infants. J Bone Joint Surg Br. 2003; 85: 115-116.
- Paul SP, Heaton PA, Patel K. Breaking it to them gently: fractured clavicle in the newborn. Pract Midwife. 2013; 16: 31-34.
- Högberg U, Fellman V, Thiblin I, Karlsson R, Wester K. Difficult birth is the main contributor to birth-related fracture and accidents to other neonatal fractures. Acta Paediatr. 2020; 7.