Epidemiological Profile of Patients in the Hemodynamics Unit of INC Hospital
- 1. Biomedical Scientist, Neurological Institute of Curitiba, INC Hospital, Curitiba, Paraná, Brazil
- 2. INC 3D Technology Lab, Neurological Institute of Curitiba, INC Hospital, Curitiba, Paraná, Brazil
- 3. Neurologist, Neurological Institute of Curitiba, INC Hospital, Department of Neurology, Curitiba, Paraná, Brazil
- 4. Neurosurgeon, Neurological Institute of Curitiba, INC Hospital, Department of Neurosurgery, Curitiba, Paraná, Brazil
Abstract
Objective: To outline the epidemiological profile of patients in the Hemodynamics in a referral hospital in Curitiba, Paraná, Brazil. Interventional neuroradiology is crucial in the management of cerebrovascular diseases, offering minimally invasive methods to diagnose and treat conditions such as aneurysms, arteriovenous malformations, carotid atherosclerotic disease, and other conditions. However, there is a lack of studies on the epidemiological profile of patients who undergo these procedures.
Methodology: Cross-sectional, retrospective study based on secondary data of neurovascular procedures performed between 2008 and 2024 at the Hemodynamics of INC Hospital. The following variables were analyzed: age, gender, health insurance, and type of procedure, using descriptive statistics in Excel®.
Results: The sample included 4607 patients, with a mean age of 52 years (± 16.21). The majority (55.6%, n = 2559) were in the 30-59 age group, followed by patients over 60 years of age (35%, n = 1613). Women (61.88%, n = 2851)) predominated over men (38.12%, n = 1756). Regarding the paying source, 92.73% (n
= 4272) of the patients had health insurance and 7.27% (n = 335) private resources. Cerebral arteriography was the most frequent procedure (72.43%, n = 3337), followed by aneurysm treatment (10.29%, n = 474) and carotid angioplasty (8.14%, n = 375).
Discussion: The results show that the procedures are mostly performed in adults, although the elderly represent a significant portion. The prevalence of cerebral arteriography highlights its importance in clinical diagnosis. These findings are fundamental for understanding the epidemiological profile, contributing to the strategic planning and optimization of hospital resources aimed at the treatment of cerebrovascular diseases.
Keywords
- Neurosurgery
- Hemodynamics
- Epidemiology
- Interventional Radiology
Citation
da Silva JF, Dering LM, Pedro MKF, Leal AG, de Meneses MS (2025) Epidemiological Profile of Patients in the Hemodynamics Unit of INC Hospital. Ann Public Health Res 12(2): 1141.
ABBREVIATIONS
AVMs: Arteriovenous Malformations; ISAT: International Subarachnoid Aneurysm Trial Study; INC: Neurological Institute Of Curitiba Hospital.
INTRODUCTION
Interventional radiology aims to develop and implement minimally invasive techniques for the diagnosis and treatment of various diseases [1]. It is a specialty that provides unique access and treatment options for numerous cerebrovascular diseases. Currently, it is indispensable for neurological and cerebrovascular centers worldwide, having revolutionized the management of cerebrovascular disorders, particularly ischemic stroke, aneurysms, and Arteriovenous Malformations (AVMs) [2]. In 2013, approximately 26 million patients survived stroke, while 6.5 million deaths were recorded, underscoring these concerns [3]. Pathologies associated with stroke, such as extracranial atherosclerotic disease and aneurysms, can be diagnosed and treated using interventional neuroradiology techniques. Among the procedures commonly performed in this context are aneurysm treatment, angioplasties, fistula embolizations, and thrombectomies [4].
Endovascular techniques for the treatment of intracranial aneurysms include aneurysm coiling, with or without adjunctive techniques such as balloon inflation or stent placement in the aneurysm neck in cases of unfavorable neck anatomy, the use of flow diverters, and flow disruptors [5]. According to the International Subarachnoid Aneurysm Trial (ISAT) study, a randomized, multicenter clinical trial that compared surgical clipping with coil embolization in patients with ruptured cerebral aneurysms in the anterior circulation, the probability of being alive with a good outcome, compared to death or dependence, was significantly better in the embolized group [6]. Furthermore, the durability and clinical benefit of embolization, observed after one year, are maintained after ten years [7].
For revascularization in extracranial atherosclerotic disease, endovascular therapies offer a plausible treatment strategy, being effective in restoring blood flow and reversing hemodynamic insufficiency [8,9]. Submaximal angioplasty demonstrated an overall technical success rate of 93% in patients with intracranial atherosclerotic stenosis, with stenoses reduced from 50%-80% to less than 20% [10]. The efficacy of percutaneous transluminal angioplasty with stent placement, compared to patients treated with aggressive medical management alone, is still an active area of investigation [11], as studies have not found a significant reduction in stroke risk in patients who underwent angioplasty with stent placement [12].
Identifying the causes of death and morbidity in a population is essential for improving the quality of life of society [13]. Furthermore, epidemiological investigations can contribute to improved healthcare delivery, service organization, and protocol optimization [14]. However, currently, the literature lacks studies on the epidemiological profile of patients undergoing this type of interventional procedure. Given the growing utilization of these techniques, there is an increasing need to understand the epidemiology of patients undergoing these interventions, analyzing factors such as sex, age group, frequency, and specific characteristics of the procedures.
In this context, the present study aims to establish an epidemiological profile of patients from the Neurological Institute of Curitiba (INC) Hospital, Curitiba, Parana, Brazil, undergoing hemodynamic procedures of interventional neuroradiology.
MATERIALS AND METHODS
This study is characterized as a cross-sectional, retrospective study based on secondary data, conducted through the analysis of medical records of patients who underwent neurointerventional procedures in the Hemodynamics Department between 2008 and 2024 at INC Hospital, located in Curitiba, Paraná.
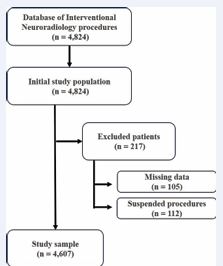
The initial population of this study comprised 4,824 patients treated by the Hemodynamics Department of INC Hospital, specifically by interventional neuroradiology. The study sample consisted of patients who underwent cerebral arteriography, peripheral angiography, angioplasty (of the carotid, vertebral, subclavian, basilar, and middle cerebral arteries), treatment procedures (for aneurysms, AVMs, tumors, dural arteriovenous fistulas, and meningeal artery for subdural hematomas), as well as patients who underwent thrombectomy and thrombolytic enzyme infusion. Patients with missing data regarding age, procedure date, procedure name, procedure report, and health insurance information were excluded. Additionally, data from suspended procedures were excluded. Finally, after applying the inclusion and exclusion criteria, the present study evaluated a sample of 4,607 participants. The flowchart (Figure 1) summarizes the participant selection process.
The data used were obtained from existing hospital records (secondary data), without direct contact with patients, and were anonymized prior to analysis to ensure patient confidentiality and privacy. The study was approved by the Research Ethics Committee of the institution, under CAAE number 88183325.1.0000.5227.
Figure 1 Sample Selection Flowchart.
RESULTS AND DISCUSSION
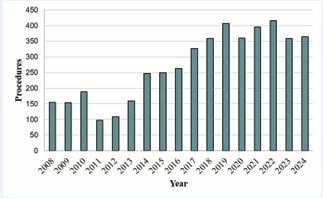
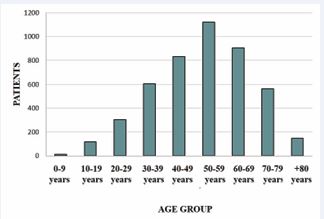
The final sample comprised 4,607 patients, and over the years, the number of procedures performed in the Hemodynamics Department per year increased (Figure 2). The sample presented a mean age of 52 years (± 16.21), with a higher concentration of patients between 30 and 59 years old (55.6%, n = 2,559), followed by patients aged 60 years or older (35%, n = 1,613) (Figure 3). The distribution by sex showed that 38.12% (n = 1,756) were male and 61.88% (n = 2,851) were female, indicating the prevalence of female patients (Table 1).
Figure 2 Total of procedures per year.
Figure 3 Age group of the sample.
Table 1: Patients sex.
|
Sex |
Relative frequency |
Absolute frequency |
|
F |
61.88% |
2851 |
|
M |
38.12% |
1756 |
Regarding the patients’ payment source, the majority were covered by health insurance (92.73%, n = 4,272). Only 7.27% (n = 335) of patients underwent the procedure with own resources. Concerning the procedures performed, the most frequent was cerebral arteriography (72.43%, n = 3,337), a procedure classified as diagnostic, followed by aneurysm treatment (10.29%, n = 474) and carotid artery angioplasty (8.14%, n = 375), AVM embolization (2.87%, n = 132), thrombectomy (1.74%, n = 80), vertebral artery angioplasty (1.19%, n = 55), and tumor embolization (1.28%, n = 59). Data on less frequent procedures, as well as those mentioned above, are presented in (Table 2).
Table 2: Procedures performed.
|
Procedure |
Relative frequency |
Absolute frequency |
|
Cerebral arteriography |
73.74% |
3397 |
|
Aneurysm treatment |
10.29% |
474 |
|
Carotid artery angioplasty |
8.14% |
375 |
|
AVM embolization |
3.06% |
141 |
|
Thrombectomy |
1.74% |
80 |
|
Vertebral artery angioplasty |
1.19% |
55 |
|
Tumor embolization |
1.28% |
59 |
|
Thrombolytic therapy |
0.39% |
18 |
|
Subclavian artery angioplasty |
0.11% |
5 |
|
Intracranial artery angioplasty |
0.07% |
3 |
Regarding angioplasties, 59.36% (n = 260) of patients were male and 40.64% (n = 178) were female. The mean age of patients who underwent angioplasty was 68 years (± 12.74). Concerning the methods used to perform the procedure, the most frequent was the use of filter, stent, and balloon (49.74%, n = 209), followed by balloon and stent (32.47%, n = 139), and stent alone (12.71%, n = 67). Other methods used were filter and stent (2.24%, n = 10), balloon alone (1.67%, n = 8), and expandable stent and balloon (1.16%, n = 5). Regarding aneurysm treatment, 78.48% (n = 372) of patients were female, while only 21.52% (n = 102) were male. The mean age of patients who underwent aneurysm treatment was 54 years (± 13.10). Concerning the methods used, the most frequent was flow diverter (56.12%, n = 266), followed by microcoils (standalone) (24.05%, n = 114), remodeling (10.97%, n = 52), stent-assisted (6.12%, n = 29), and flow disruptor (2.74%, n = 13) (Table 3). Among flow diverters, the more used was FRED (93,98%, n = 250), followed by SILK (1,88%, n = 5), PIPELINE (1,88%, n = 5), FRED Jr. (1,51%, n = 4), and DERIVO (0,75%, n = 2).
The results of this study enabled us to delineate the epidemiological profile of patients undergoing interventional neuroradiology procedures in the Hemodynamics Department of Hospital INC, revealing patterns relevant to clinical practice and health facilities planning. The analyzed sample comprised 4,607 patients, with a predominance of female patients (61.88%) and a mean age of 52 years, with the main concentration in the age range between 30 and 59 years. These data suggest a service pattern directed primarily toward the adult population, especially female patients, which may reflect both the distribution of clinical demand and the demographic profile of the served population. The vast majority of patients were covered by health insurance plans (92.73%), with the remainder receiving self-funding care (7.27%). This profile is directly related to the nature of the institution, which performs procedures only for patients with health insurance or private care coverage; therefore, the epidemiological profile outlined here represents only a specific portion of the population, possibly with greater access to early diagnosis and specialized treatments.
The most frequently performed procedure was cerebral arteriography (72.43%), of a diagnostic nature, indicating the importance of this examination in the initial evaluation of patients. Among therapeutic procedures, aneurysm treatment (10.29%) and carotid artery angioplasty (8.14%) stand out. The specific analysis of interventions reveals important particularities: patients undergoing angioplasty, regardless of the artery, presented a higher mean age (68 years) and a predominance of male patients (59.36%), which is consistent with the literature on atherosclerosis, a condition more prevalent in men and at more advanced ages [15,16]. Conversely, aneurysm treatment was predominant in female patients (78.48%), with a mean age of 54 years, findings that agree with the demographic characteristics described in previous studies on the prevalence of intracranial aneurysms, which are usually more frequent in women over 30 years of age [17].
Although specific epidemiological studies for direct comparison were not found, the data presented contribute to filling a gap in the literature and may serve as a foundation for future investigations in the field. The characteristics observed in the profile of the studied population reinforce the importance of considering the local context in resource planning and service delivery strategies. Furthermore, the findings indicate potential risk groups or those with greater demand for procedures, which can guide more effective interventions, both preventive and therapeutic. This study has limitations regarding the fact that it is retrospective and based on a database filled by health service employees, susceptible to missing information or completion errors. However, cases with identified flaws that were not amenable to correction were excluded from the analyzed sample. Furthermore, by using patients from only a single hospital located in a large center such as the city of Curitiba, it probably does not reflect the epidemiological profile of the Brazilian population as a whole, given its vast size and diversity of healthcare services. The present study did not evaluate the analysis of clinical outcomes or post-procedure patient follow-up, important information for understanding the efficacy and safety of the procedures performed. Nevertheless, the sample size and the rigor in data analysis strengthen the validity of the results.
Further studies may analyze more characteristic data of each procedure, for example, the methods used for AVM embolization, fistulas and tumors, the location of aneurysms, the quantity of each material used, and other relevant information for each procedure. Future studies should also analyze aspects of patient clinical outcomes, in addition to considering multicenter approaches and more robust analyses, such as comparative models between variables, to deepen the understanding of the determinants of the analyzed procedures and their outcomes.
Table 3: Métodos utilizados no tratamento de aneurismas.
|
Método |
Frequência relativa |
Frequência absoluta |
|
Diversor de fluxo |
56,12% |
266 |
|
Micromolas (solo) |
24,05% |
114 |
|
Remodeling |
10,97% |
52 |
|
Stent-assisted |
6,12% |
29 |
|
Disruptor de fluxo |
2,74% |
13 |
CONCLUSION
The present study enabled us to delineate the epidemiological profile of the population served at INC Hospital during the period from 2008 to 2024. It was observed that neurointerventional procedures are predominantly performed in adults, although elderly patients represent a significant portion of the care provided, and cerebral arteriography is the most frequent procedure, highlighting the importance of diagnosis in clinical practice. The distribution by sex demonstrated that female patients are predominantly treated by interventional neuroradiology, although this distribution varies according to the type of procedure performed. These results contribute to the understanding of the clinical and demographic characteristics of this population, providing support for planning more targeted and effective health actions. Furthermore, the data obtained reinforce the importance of studies that evaluate the pattern of care and clinical outcomes, aiming at improving the quality of services provided. For future studies, we recommend conducting new investigations, preferably performing multicenter studies with greater analytical depth, to validate the findings and expand the knowledge on the subject.
REFERENCES
- Maingard J, Kok HK, Ranatunga D, Brooks DM, Chandra RV, Lee MJ, et al. The future of interventional and neurointerventional radiology: learning lessons from the past. Br J Radiol. 2017; 90: 20170473.
- Pelz DM, Lownie SP, Mayich MS, Pandey SK, Sharma M. Interventional Neuroradiology: A Review. Can J Neurol Sci. 2021; 48: 172-188.
- Kompoliti K, Doumbe J, Mapoure YN, Nyinyikua T, Ouyang B, Shah H, et al. Mortality and morbidity among hospitalized adult patients with neurological diseases in Cameroon. J Neurol Sci. 2017; 381: 165-168.
- Calixte A, Lartigue S, McGaugh S, Mathelier M, Patel A, et al. Neurointerventional Radiology: History, Present and Future. J Radiol Oncol. 2023; 7: 026-032.
- Ajiboye N, Chalouhi N, Starke RM, Zanaty M, Bell R. Unruptured Cerebral Aneurysms: Evaluation and Management. ScientificWorldJournal. 2015: 2015: 954954.
- Molyneux AJ, Kerr RS, Yu LM, Clarke M, Sneade M, Yarnold JA, et al. International subarachnoid aneurysm trial (ISAT) of neurosurgical clipping versus endovascular coiling in 2143 patients with ruptured
intracranial aneurysms: a randomised comparison of effects on survival, dependency, seizures, rebleeding, subgroups, and aneurysm occlusion. Lancet. 2005; 366: 809-17.
- Molyneux AJ, Birks J, Clarke A, Sneade M, Kerr RS. The durability of endovascular coiling versus neurosurgical clipping of ruptured cerebral aneurysms: 18 year follow-up of the UK cohort of the International Subarachnoid Aneurysm Trial (ISAT). Lancet. 2015 ; 385: 691-7.
- Prabhakaran S, Wells KR, Jhaveri MD, Lopes DK. Hemodynamic changes following wingspan stent placement--a quantitative magnetic resonance angiography study. J Neuroimaging. 2011; 21: e109-13.
- Guppy KH, Charbel FT, Corsten LA, Zhao M, Debrun G. Hemodynamic evaluation of basilar and vertebral artery angioplasty. Neurosurgery. 2002; 51: 327-334.
- Seyedsaadat SM, Yolcu YU, Neuhaus A, Rizvi A, Alzuabi M, Murad MH, et al. Submaximal angioplasty in the treatment of patients with symptomatic ICAD: a systematic review and meta-analysis. J Neurointerv Surg. 2020; 12: 380-385.
- Gutierrez J, Turan TN, Hoh BL, Chimowitz MI. Intracranial atherosclerotic stenosis: risk factors, diagnosis, and treatment. Lancet Neurol. 2022; 21: 355-368.
- Lutsep HL, Barnwell SL, Larsen DT, Lynn MJ, Hong M, Turan TN, et al. Outcome in patients previously on antithrombotic therapy in the SAMMPRIS trial: subgroup analysis. Stroke. 2015; 46: 775-779.
- Deuschl G, Beghi E, Fazekas F, Varga T, Christoforidi KA, Sipido E, et al. The burden of neurological diseases in Europe: an analysis for the Global Burden of Disease Study 2017. The Lancet Public Health. 2020; 5: e551–e567.
- Barros FLOS, Carvalho KMMB, Falcão ARN, Ribeiro Filho JDM, Gadelha RRM, Campos DCO. Perfil epidemiológico dos pacientes atendidos em uma unidade de terapia intensiva cardiopulmonar de um hospital de referência do Ceará. Revista de Medicina da UFC, Fortaleza, 2020; 60: 26-30.
- Song JY, Kwon SU. Intracranial Atherosclerotic Stenosis. Cerebrovasc Dis Extra. 2025; 15: 62-67.
- Wang Y, Zhao X, Liu L, Soo YO, Pu Y, Pan Y, et al. Prevalence and outcomes of symptomatic intracranial large artery stenoses and occlusions in China: the Chinese Intracranial Atherosclerosis (CICAS) Study. Stroke. 2014; 45: 663-669.
- Vlak MH, Algra A, Brandenburg R, Rinkel GJ. Prevalence of unruptured intracranial aneurysms, with emphasis on sex, age, comorbidity, country, and time period: a systematic review and meta-analysis. Lancet Neurol. 2011; 10: 626-636.