Omega3 Fatty Acids: Do They Raise Health Concerns?
- 1. Department of Biochemistry, Amala Cancer Research Centre (recognized by University of Calicut), Amala Nagar, Thrissur, Kerala, India
Abstract
A volume of epidemiological, experimental and clinical data reveals the beneficial effect of omega 3 class of fatty acids in a variety of human ailments. However, conflicting results do exist and long term use of these highly unsaturated fatty acids has been cautioned due to its susceptibility to oxidative changes. Enzymatic oxidation of well-known omega 3 fatty acids docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA) is known to produce 4-hydroxy 2-hexanal (4-HHE), an alpha beta unsaturated aldehyde. The molecule has been shown to protect endothelial cells through Nuclear factor related erythroid factor 2 (Nrf2) mediated HO-1 expression while induce toxicity in neuronal cells. Also high levels of HHE protein adducts are reported in neuronal degenerative tissues. Therefore, it is likely that omega 3 fatty acids may have detrimental effect rather than beneficial effects when cellular/tissue redox status as well as fatty aldehyde detoxification system is challenged. The present review aims to open up a discussion on the possible health concerns upon long term consumption of omega3 fatty acids.
Keywords
Omega 3 fatty acids; Enzymatic oxidation; 4-HHE; Oxidative stress; Ageing.
CITATION
Narayanankutty A, Vakayil M, Manalil JJ, Ramavarma SK, Suseela IM, et al. (2016) Omega3 Fatty Acids: Do They Raise Health Concerns? JSM Biochem Mol Biol 3(1): 1016.
ABBREVIATIONS
NRF2: Nuclear factor erythroid 2-related factor 2; 4-HHE 4: Hydroxy 2 Hexenal; HO-1: Heme Oxygenase 1; DHA: Docosahexaenoic Acid; EPA: Eicosapentaenoic Acid
INTRODUCTION
Omega 3 fatty acids are essential poly unsaturated fatty acids of high therapeutic value. Several epidemiological, experimental and clinical studies have brought light to the health effects of these molecules [1-20], (Table 1).
|
Table 1: Health benefits of omega 3 fatty acids. |
|||
|
Effect |
Mechanism |
Author |
Year |
|
Cardiovascular diseases and lipid metabolism |
Omega 3 fatty acids and their role in vascular endothelial tissues |
Zanetti, Grillo [1] |
2015 |
|
Relaxation of the vascular smooth muscles by stimulating the nitric oxide synthesis from endothelial cells |
Loscalzo [2] |
2013 |
|
|
Promoting endothelial repair and reducing plasma lipids. It is also likely that the replacement of saturated fatty acids from cell membranes of cardiomyocytes for omega 3 fatty acids may account for the antiarrhythmic effect with an average decrease of 5.8 and 3.3 mm Hg for systolic and diastolic blood pressure |
Mori and Woodman [3]
|
2006
|
|
|
DHA changes the distribution of LDL particle sub-fractions in favor, of less atherogenic, large, buoyant LDLs |
Mori, Burke [4]
|
2000 |
|
|
Omega 3 fatty acids as therapeutic options for hypertriglyceridemia |
Ito [5] |
2015 |
|
|
Omega 3 fatty acids promote macrophage reverse cholesterol transport in high fat fed hamsters |
Kasbi Chadli, Nazih [6] |
2015 |
|
|
Reduce TAG production by increasing fatty acid oxidation via peroxisomal β-oxidation |
Vrablik, Prusikova [7] |
2009 |
|
|
Reduce plasma concentration of fibrinogen |
Vanschoonbeek, Feijge [8] |
2004 |
|
|
Cancer progression and metastasis |
Breast cancer and metastasis |
Chamras, Ardashian [9] Abdi-Dezfuli, Froyland [10] |
2002
1997 |
|
DHA and EPA inhibit pancreas cancer cell growth by down regulating Wnt/beta–catenin signaling |
Corsetto, Montorfano [11] |
2011 |
|
|
Omega 3 fatty acids down regulate malignancy potential of colon cancer cells |
Cockbain, Volpato [12] Chamberland and Moon [13] |
2014
2014 |
|
|
Omega 3 fatty acid and their implications in multi targeted cancer therapy |
D’Eliseo and Velotti [14] |
2016 |
|
|
Omega 3 fatty acids in management of gastrointestinal cancer |
Eltweri, Thomas [15] |
2016 |
|
|
Neurodegeneration |
Supplementation of DHA results in neuro protection in Parkinson’s disease |
Bousquet, Gue [16] |
2011 |
|
Reduce neuro-inflammation through GPR120 mediated mechanism |
Wellhauser and Belsham [17] |
2014 |
|
|
Non esterified DHA increase levels of neuro protection D1 Omega 3 fatty acid induce cerebral angiogenesis to provide long term protection for neurons |
Orr, Palumbo [18]
Wang, Shi [19] |
2013
2014 |
|
|
Omega 3 fatty acids as adjuvant s for Alzheimer’s disease treatment |
Casali, Corona [20] |
2015 |
|
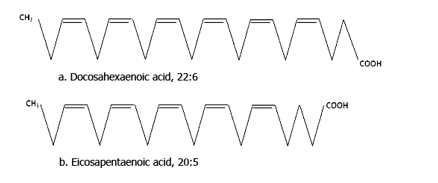
Among the various class of compounds, long chain unsaturated docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA) are the most studied (Figure 1 a and b).
Figure 1: Structure of two common omega 3 fatty acids; docosahexaenoic acid (a) and Eicosapentaenoic acid (b).
Currently EPA and DHA together with vitamin E have been in market and 2-3g daily dose has been used for the treatment of familial hypertriglyceridemia, psychological disorders and other neurodegenerative conditions [21,22]. It is claimed that omega 3 fatty acid tablets bring down the TG level to 500 mg dL in familial triglyceridemia patients having 2000 mg/dL TG in their blood. However, other medications are also needed to reduce the level of TG to almost near normal. Eventhough, recent studies have reported the possible health hazards of an aldehyde oxidation products of omega 3 fats, 4-hydroxy hexenal. The pro inflammatory and toxic insults of these aldehyde molecules thus raise concern over the long term use of these essential fatty acids.
Mechanistic basis for the biological effect of Omega 3 fatty acids
When very long chain omega 3 fatty acids are ingested, there is high incorporation of EPA and DHA into membrane phospholipids at the expense of arachidonic acid (AA) [23,24], which may alter the physical characteristics of cell membrane [25], and affects the function of cells. In vitro studies have demonstrated that replacement of omega-6 fatty acids with omega 3 fatty acids may cause a decreased cellular response to mitogenic and inflammatory stimuli via reduced proliferation of inflammatory cells, expression of Cox-2 and release IL-6 due to lower generation of PGE2 than PGE3 [26].
It has been also reported that omega 3 fatty acid change the lipid raft composition thereby decreasing epidermal growth factor receptor expression in breast cancer cells [25], suggesting a possible mechanism of inhibition of cell proliferation. The use of these polyunsaturated fats as an adjuvant in chemotherapy is also suggested [27]. However, in cancer prevention or chemotherapy, the benefits have been limited to the improvement in quality life of patients [28], and even some studies raised concerns of being developing drug resistance [29].
The recent information on the anti-tumour properties of omega 3 fatty acid relies on its oxidative stress inducing potential Mechanistic basis for the biological effect of Omega 3 fatty acids When very long chain omega 3 fatty acids are ingested, there is high incorporation of EPA and DHA into membrane phospholipids at the expense of arachidonic acid (AA) [23,24], which may alter the physical characteristics of cell membrane [25], and affects the function of cells. In vitro studies have demonstrated that replacement of omega-6 fatty acids with omega 3 fatty acids may cause a decreased cellular response to mitogenic and inflammatory stimuli via reduced proliferation of inflammatory cells, expression of Cox-2 and release IL-6 due to lower generation of PGE2 than PGE3 [26]. It has been also reported that omega 3 fatty acid change the lipid raft composition thereby decreasing epidermal growth factor receptor expression in breast cancer cells [25], suggesting a possible mechanism of inhibition of cell proliferation. The use of these polyunsaturated fats as an adjuvant in chemotherapy is also suggested [27]. However, in cancer prevention or chemotherapy, the benefits have been limited to the improvement in quality life of patients [28], and even some studies raised concerns of being developing drug resistance [29]. The recent information on the anti-tumour properties of omega 3 fatty acid relies on its oxidative stress inducing potential AKT localization. This result in arrest of cell growth, proliferation and thereby induce apoptosis.
Risks
Apart from these beneficial effects, contradictory results also exist. High doses of omega 3 fatty acids used in the treatment of hyper triglyceridemia, LDL levels rise by 10%, this effect being even more pronounced in patients with extreme TG elevations at baseline [36]. DHA, not EPA has been reported to cause this adverse effect. However, it has been claimed that increase in the LDLc fraction during omega 3 fatty acid intake may not be hazardous as they are beneficial in nature. But, as omega 3 fatty acid are prone to oxidative modifications, their increase in LDLc may lead a subsequent hike in oxidized LDL, which is a known risk factor for atherogenesis and other lipid related disorders. Substantiating this assumption, studies by Whitman, Fish [37], demonstrated that incorporation of omega 3 fatty acid in an atherogenic diet increased the LDL oxidation in vitro. Several other studies suggests the increased risk of type 2 diabetes mellitus during the high omega 3 fatty acid intake [38].
Center for Food Safety and Applied Nutrition, USA has reported the known as well as suspected risks of docosahexaenoic acid and eicosapentaenoic acid consumption in excess of 3 grams per day. It includes the possibility of increased incidence of bleeding, hemorrhagic stroke, oxidative modifications of these fatty acid molecules into biologically active signaling molecules, elevated apoproteins levels which are associated with LDL cholesterol and reduced glycemic control among diabetic and hyperlipidemics.
The immediate oxidation products of omega 3 fats are epoxides, peroxides and aldehydes, which are known to be involved in oxidative stress and damages. Trans 4-hydroxy hexenal (HHE) is a product of omega 3 fatty acid oxidation similar to hydroxy nonenal (HNE) omega 6 fat derivative [39], and have roles as an active biochemical mediator. Recent reports by Calzada, Colas [40], shown that consumption of unoxidized DHA over a period of 8 weeks increase the serum levels of 4-HHE. Further, gastrointestinal digestion of fish and cod oils resulted in the formation and accumulation of HHE and other lipid derived aldehydes including malondialdehyde as well as HNE in the intestinal lumen [41,42]. Few studies have reported the beneficial effects of HHE in oxidative signaling by inducing Nrf2 mediated heme oxygenase 1 expression in the vascular endothelial cells [43]. Later studies in animals (C57BL/6mice) also observed similar results by Ishikado, Morino [44]. The implication of these results as a beneficial effect of HHE may not be accurate as the hike in Nrf2 could be only temporary in order to detoxify HHE. Overwhelming production of HHE for long duration may not support by short term hike in Nrf2expression. Further studies are needed to understand the dose dependent expression and duration of Nrf2 offering cytoprotection under HHE challenge to clarify this assumption.
It has also been reported that exposure HHE to human and murine vascular endothelial cells elevate Monocyte chemotactic protein (MCP-1), which is a proinflammatory molecule [45]. There are also reports that HHE induce p38 MAP kinase expression and thereby increase pro-inflammatory activity by up regulating the expressions of NF-kB, cyclooxygenase and inducible nitric oxide synthase. The study suggests that these mechanisms promote epithelial mesenchymal transition in renal tubular epithelial cell, HK-2 [46]. Similar observations have also been made by Bae, Joo [47], where HHE found to induce inflammatory gene expression with concomitant reduction in Nrf2 based antioxidant defense in kidney cells. Supporting the above, Lee, Je [48], reported that HHE induces pro-inflammatory cytokine expression and apoptosis in vascular endothelial cells. In rats fed with oxidized omega 3 fatty acids, increased accumulation of HHE in blood has been reported, which in turn resulted in the increase in serum inflammatory markers such as NF-kB and oxidative stress marker glutathione peroxidase expression in intestinal tissues [49]. Similar results are shared by Bradley, Xiong-Fister [50], as HHE-protein adducts are elevated in several of the neurodegenerative disorders, which is an independent risk factor for the progression of these disorders. In addition to these, a latest study by Grimm, Haupenthal [51], indicated that oxidized DHA exposure to cortical neuronal cells increases the levels of β-amyloid peptide and amyloidogenic amyloid precursor protein (APP), which are involved in the progression of neurodegenerative disorders including Alzheimer’s disease. HHE has also been shown to be neurotoxic in primary cell cultures mediated through GSH depletion [52]. Since the oxidized products of omega 3 fats, such as HHE can induce proinflammatory condition in the body and precipitate in neuronal degeneration, long term consumption of omega 3 fats need to be reconsidered.
Fatty aldehyde dehydrogenases and aldehyde detoxification
However, aldehydes such as HHE are usually detoxified by a well-defined aldehyde detoxification system in the body. These include aldehyde oxidase, aldehyde keto-reductase and aldehyde dehydrogenase. Fatty aldehyde dehydrogenase (or long-chain aldehyde dehydrogenase), belong to the oxidoreductase family of NAD(P)+-dependent enzymes are encoded in the ALDH3A2 gene on chromosome-17 is an aldehyde dehydrogenase enzyme that remove toxic aldehydes generated by the metabolism of alcohol and lipid peroxidation. GSH which can form adducts with aldehydes and enhance their removal are the determining factor of this secondary oxidative and carbonyl stress. The ectopic expression of FALDH significantly decreased ROS production in cells treated by 4-hydroxynonenal (4-HNE), suggesting that FALDH protects against oxidative stress associated with lipid peroxidation [53]. Further, it has been reported that polyunsaturated fatty acids up regulate the expression of fatty aldehyde dehydrogenase mediated by PPAR alpha, in order to reduce the oxidative stress induced by the aldehydes derived from these fatty acids [54].
It is considered that in young individual, endogenous antioxidant system and fatty aldehyde dehydrogenases are sufficient to protect against oxidative stress and protein carbonyl adduct formation. However in individuals, where the antioxidant system is challenged, the detoxifying system may also be dysfunctional due to overwhelming carbonyl molecules [55]. Similar condition prevail during aging where a higher incidence of several diseases including dementia, Parkinson’s disease, diabetes, cancer, and Alzheimer’s diseases are reported [56-58]. There need more studies to see whether these population can be benefited from omega 3-fat consumption.
CONCLUSION
Despite the reported benefits of omega 3 fatty acids, there arise concerns that long term consumption may lead to deleterious effect in the body. This is mainly because of the emerging reports that oxidation of omega 3 fatty acid generates toxic aldehydes such as 4-hydroxy 2-hexenal which may cause chronic inflammation and also forms adducts with cellular macromolecules, eventually contributing to degenerative disease pathology. Therefore, it is suggested that the safety of these fatty acids in long term consumption need to be ensured.
ACKNOWLEDGEMENTS
Corresponding author acknowledge Indian Council of Medical Research (ICMR) for the financial assistance (Research Ad-hoc scheme No. BMS/Adhoc/25/2012-2013, File No: 52/16/2011 BMS). Arunaksharan Narayanankutty is thankful to the Council of Scientific and Industrial Research (CSIR-HRDG), India for the financial support in the form of Senior Research Fellowship (09/869 (0012)/2012-EMR-I).