Multidrug-Resistant Mycoplasma genitalium presenting with purulent urethral discharge mimicking Gonorrhoea
- 1. Integrated Sexual Health Services, Rotherham Hospital, United Kingdom
Citation
Anim-Addo N (2021) Multidrug-Resistant Mycoplasma genitalium presenting with purulent urethral discharge mimicking Gonorrhoea. JSM Clin Case Rep 9(1): 1183.
INTRODUCTION
We describe a case of Mycoplasma genitalium infection in a male presenting with purulent urethral discharge that mimicked the presentation of Gonorrhoea. A recent study estimated the prevalence of M. genitalium in those aged between 16 - 44 to be similar to that of Chlamydia trachomatis [1].Despite considerable prevalence, provisions for testing are not routinely available in all UK Sexual Health clinics.
CASE REPORT
A 23-year-old male presented with a 4-week history of persistent dysuria and creamy yellow discharge despite completion of treatment for Non-Gonococcal Urethritis (NGU) initiated by another Sexual Health clinic. He had refrained from sexual intercourse during and following his treatment. Microscopy was repeated and confirmed NGU for a second time. Chlamydia trachomatis and Neisseria gonorrhoeae NAAT were both negative, and a urine culture confirmed sterile pyuria. The clinical appearance of the urethral discharge was thought to be typical of N. Gonorrhoeae and it was felt that his recent treatment at the previous Sexual Health clinic may have led to false-negative results.
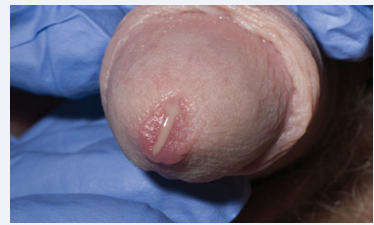
First-line treatment with Doxycycline failed to improve his symptoms. He was treated again, in accordance with British Association of Sexual Health and HIV (BASHH) NGU guidance, for recurrent / persistent NGU with a 3-day course of Azithromycin in addition to a 5-day course of Metronidazole. This led to only a transient improvement of his symptoms, and the discharge returned, although to a lesser degree (Figure 1).
Figure 1 Purulent urethral discharge caused by M. genitalium.
Urine M. genitalium PCR was requested and was positive. Macrolide resistance-associated mutations were also identified. A 10-day course of Moxifloxacin resulted in complete resolution of symptoms. His current sexual partner was also tested and treated with Moxifloxacin, and a test of cure 5 weeks later was negative.
DISCUSSION
M. genitalium is a fastidious bacterium that invades epithelial cells of the urogenital tract and is transmitted through sexual contact [2]. M. genitalium cannot replication [2,3]. BASHH recommendations are that PCR testing be performed in specific circumstances, such as all cases of NGU [3]. However, M. genitalium testing is still not widely available in the UK and macrolide resistance testing remains cost-prohibitive in many clinics. Despite BASHH recommendations, a survey of 125 public health commissioners found that only one in ten were making provisions for M. genitalium testing [4].
M. genitalium is a prevalent STI and burgeoning antibiotic resistance is proving challenging, with macrolide resistance estimated at 40% [3]. Diagnostic testing for M. genitalium in the UK remains relatively expensive unlike its counterparts in prevalence, N. gonorrhoeae and C. trachomatis. With the lack of availability of optimal testing, it can be assumed that M. genitalium is considerably under-diagnosed and also incidentally suboptimally treated in patients tested and treated for other asymptomatic STIs. Patients may experience transient improvement in symptoms if treated with doxycycline alone in cases of NGU if the M. genitalium species is macrolide sensitive. Deficient provision for PCR testing leads to inadequately tailored antibiotic regimens and further antibiotic resistance. Significant levels of antibiotic resistance results in an increase in cases of treatment failure and a dwindling reserve of antibiotics able to achieve complete resolution of symptoms and clearance of infection.