Facial Prosthesis using an Acrylic Base for a Patient with a Large Facial Defect
- 1. Department of Maxillofacial Prosthetics, Tokyo Medical and Dental University, Japan
Abstract
This case report describes the fabrication of a prosthesis for the rehabilitation of an elderly male patient with a large facial defect after mandibulectomy. After surgical resection, the patient’s defect involved the lower lip and cheek and connected to the oral cavity. The surgeons desired a prosthetic solution to improve speech, mastication, deglutition, and esthetics. An acrylic base (Palapress vario clear; Heraeus-Kulzer, Japan) with wires was fabricated to support a silicone facial prosthesis that matched his skin color. This facial prosthesis was fabricated from maxillofacial silicone material with intrinsic color and covered the acrylic surface. A silicone facial prosthesis could be a solution for rehabilitation in elderly patients with a large facial defect resulting from mandibulectomy.While prosthetic treatment is an option for improving dysfunction and esthetic problems following mandibulectomy, surgical planning must be carefully considered and collaborative efforts are needed from the preoperative planning stage.
Keywords
• Facial prosthesis
• Mandibulectomy
• Cancer
• Facial defect
• Planning
Citation
Sumita YI, Hattori M, Shigen Y, Taniguchi H (2016) Facial Prosthesis using an Acrylic Base for a Patient with a Large Facial Defect. JSM Dent Surg 1(1): 1006.
ABBREVIATIONS
QOL: Quality of Life
INTRODUCTION
Facial surgical defects can affect patients’ orofacial function, esthetics, and psychological wellbeing [1], and prosthetic treatment is an option when there are limitations to full recovery with surgery alone. The retentive properties, stability, and esthetics of prosthesis often influence maxillofacial prosthetic success and help to maintain social life after the surgery [2,3], However, large defects make it difficult to achieve prosthetic retention. From the sixteenth century up to the present day, clinicians have used a variety of techniques to try to improve retention [4,5]. Prior to the operation; surgeons simulate the procedures involved and plan various options. Normally after mandibulectomy, surgical reconstruction must be considered in order to alleviate the dysfunction caused by the defect. Surgeons need to consider several options to avoid a poor outcome. Although rare, it is possible for the graft to be lost because of infection or for some other unfavorable outcome to occur. Prosthetic treatment can then be selected as an option.
This case report describes the fabrication of prosthesis for the rehabilitation of an elderly patient with a large facial defect after mandibulectomy. After surgical resection, the patient’s defect involved the lower lip and cheek, which were not reconstructed, and the resulting defect was connected to the oral cavity. After delivering a facial prosthesis with an acrylic base, the patient regained functional speech and resumed daily activities. The importance of preoperative surgical planning for providing facial prosthesis rehabilitation is discussed.
CASE PRESENTATION
An 80-year-old Japanese man had undergone left-side Mandibular resection due to squamous cell carcinoma. Mandibulectomy caused an extensive facial defect that was connected intra orally and extra orally. He could not undergo additional surgery because of complications and other surgical reasons, but details of this were missing in the referral letter from his oral surgeon. The patient was referred to us at the Maxillofacial Prosthetic Clinic at the Dental Hospital of Tokyo Medical and Dental University for prosthetic rehabilitation 2 months after the initial surgery.
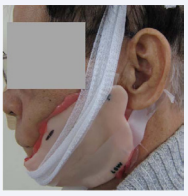
At the first visit, the defect over the left side of the face was covered with acrylic resin bordered with soft, pink-colored silicone and held in place using tape and bandage (Figures 1,2).
Figure 1: Extra-oral view of the patient on the first visiting day.
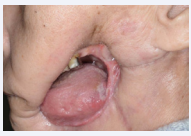
Figure 2: Extra-oral view of the facial defect before prosthetic treatment.
The surgeons decided on a prosthetic solution to improve dysfunction of speech, mastication, deglutition, and esthetics caused by the surgical resection. The most important and difficult point in planning the maxillofacial prosthetic treatment was that the facial defect involved a movable area. The structure of the defect area changed with the movements of speech and swallowing, causing difficulties with prosthesis stability.
An acrylic base (Palapress vario clear; Heraeus-Kulzer, Japan) with wires was fabricated (Figure 3) to support a silicone facial prosthesis.
Figure 3: Fabricated acrylic base.
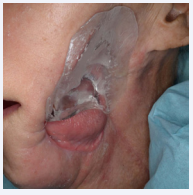
However, the patient initially had difficulty placing the acrylic base because of trismus caused by the surgery (Figure 4).
Figure 4: Extra-oral view of the patient with the acrylic base in situ.
After some instruction, he was able to successfully place it, and a facial prosthesis matching his skin color was fabricated from maxillofacial silicone material with intrinsic color (2186 Silicone Elastomer, Factor II, USA) to cover the acrylic surface. The prosthesis was fitted and retained by attachment to the peripheral skin with adhesive (Daro Adhesive Extra Strength, Factor II).
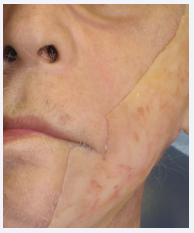
After being instructed on use of the skin adhesive, the patient was able to start using the acrylic base and silicone facial prosthesis (Figure 5).
Figure 5: Extra-oral view of the patient’s face with the acrylic base covered by the silicone facial prosthesis.
The prostheses functioned stably and allowed him to speak, swallow, and engage in social and daily activities, thereby increasing his QOL.
RESULTS AND DISCUSSION
Large facial defects typically require both surgical reconstruction and a prosthesis to restore function and esthetics. However, surgical reconstruction must be rejected in cases where it poses a high risk of failure or death. Prosthetic restoration of large facial defects involving the oral cavity can be challenging, and often involves a compromise between cosmetic versus functional adequacy. Prosthetic treatment of maxillofacial defects is reasonable from a cosmetic standpoint, but their retention always affects patient satisfaction. Retention is the most important concern for the patient [4,5] because the prosthesis needs to be used in public. If retention is not adequate, the patient will always fear that the facial prosthesis will fall. In the present case, an acrylic resin frame was used to achieve better retention from the defect area, helping to make the system more stable from the undercut. Also, there was no displacement during mouth opening, the prosthesis enabled the patient to drink without water leakage, and he could place and remove the prosthesis independently. Thus, our patient was satisfied with the functional and esthetic outcomes. The needs of individual patients should be carefully considered to determine which aspects of a prosthesis are most important for their QOL.
Despite the ultimately satisfactory outcome, the case remains a serious challenge for us. Prior to the surgical operation, if the surgeons had consulted us, it might have been possible to expand the options following mandibulectomy. The maxillofacial prosthodontist would have been able to discuss such options with the surgeons from the viewpoint of prosthetic treatment. Collaboration in a team approach is needed from the outset of treatment, during planning, to optimize patients’ QOL.
CONCLUSION
A silicone facial prosthesis could be one of the solutions for rehabilitation of elderly patients with a large facial defect resulting from Mandibulectomy.
ACKNOWLEDGEMENTS
The authors thank all our staff and patients of the Department of Maxillofacial Prosthetics, Tokyo Medical and Dental University.
This is Research was Supported by the Discreptinacy of Faculty of Dentistry at Tokyo Medical and Dental University (TMDU) to “Intractable Disease (Cancer) Unit”.