Lymphostatic Elephantiasis, Stage 3 Lymphedema in a Patient with Arteriovenous Fistulas & Arteriovenous Grafts for Hemodialysis, a Case Report
- 1. Baylor College of Medicine, Baylor St. Luke’s Medical Center, USA
- 2. Karadeniz Technical University-Faculty of Medicine, Turkey
- 3. Hamad Medical Corporation / Doha, Qatar
Abstract
Context: Lymphedema is a chronic condition of tissue swelling which occurs as a result of abnormally developed (primary lymphedema) or damaged lymphatic system (secondary lymphedema). Most of the cases are secondary and most of the secondary cases are cancer- treatment related, parasitic diseases and other etiologies including lymphedema seen in patients with ESRD.
Case: A 65-year-old man with a history of numerous arteriovenous grafts, with current dialysis access in left groin, was readmitted for increased swelling of the left leg with gait difficulties.
Conclusion: We believe that lymphedema although rare but can be one severe complication of AV fistula and whenever it is suspected, it should be treated promptly.
Keywords
• Lymphedema • Chronic edema • Lymphostatic elephantiasis • Iatrogenic lymphedema • Arteriovenous graft Arteriovenous fistula
Citation
Maher N, Orhan S, Ahmed R (2016) Lymphostatic Elephantiasis, Stage 3 Lymphedema in a Patient with Arteriovenous Fistulas & Arteriovenous Grafts for Hemodialysis, a Case Report. J Cardiol Clin Res 4(5): 1072.
CASE PRESENTATION
We describe in this case report stage 3 lymphedema in a patient on chronic hemodialysis who underwent several arteriovenous fistula (AVF) and arteriovenous graft (AVG) procedures in both arms, all failed and clotted, requiring placement of AVG in left groin. Lymphedema developed in left arm and left leg.
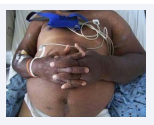
We present here a 65-year-old morbidly obese man (BMI: 37.85) with a history of numerous arteriovenous grafts (6 arteriovenous grafts in both arms -all clotted-) with current dialysis access in left groin, was readmitted for increased swelling of the left leg and gait difficulties. He has been on dialysis for 14 years for end-stage-renal-disease secondary to hypertension. Patient was treated for associated cellulitis at different times. On examination size differences between both arms (Figure 1) and legs were prominent.
Figure 1: Lymphedema involving the left upper extremity with an old AVG of Left arm.
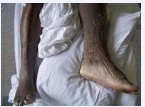
His lymphedema was stage III based on the International Society of Lymphology classification. This encompasses lymphostatic elephantiasis where pitting is absent and trophic skin changes such as acanthosis, fat deposits, and warty overgrowths develop (Figure 2).
Figure 2: Left lower extremity after aggressive dialysis with mild edema.
DISCUSSION
Lymphedema is a chronic condition of tissue swelling which occurs as a result of abnormally developed (primary lymphedema) or damaged lymphatic system (secondary lymphedema). Most of the cases are secondary and most of the secondary cases are cancer- treatment related, parasitic diseases and other etiologies including lymphedema seen in patients with ESRD.
Lymphedema occurs with physical obstruction of the lymphatic vessel lumen, either by extramural forces or intraluminal obstruction. Destruction of lymphatics by several mechanisms include valve incompetence between lymphangions, paralysis of lymphatic muscles, reduced tissue motion, diminished arterial pulsations or venomotion, and elevated venous pressure at the drainage points where lymphatics empty into the systemic blood circulation [1]. Lymphedema affects approximately 140 million people worldwide. The total crude estimated prevalence of chronic edema/lymphoedema is 1.33/1000 population [2]. The swelling and subsequent induration of the affected region can cause disfigurement, as well as decreased mobility and function [3]. Tissues with lymphedema are at risk of infection and changes are irreversible ending in lymphostatic elephantiasis.
Treatment of lymphedema is based on rerouting the lymphatic fluid through remaining functional lymph vessels. This is accomplished through elevation, exercises, compression garments/devices, and manual lymph drainage. This is usually combined with good skin care practices [4]. There are numerous risk factors for lymphedema including; obesity (as in our patient), infection and trauma. Prevention of these factors may also play a role in treatment.
This patient had many AVGs. He started to develop lymphedema after occlusion of his AVFs which may suggest additive effect on worsening of lymphedema.
We think that repeated dialysis access placement (AVFs/ AVGs) on the same side plays a role in development and progression of lymphedema.
CONCLUSION
Hemodialysis and AVG procedures are common in clinical practice. Lymphedema is uncommon but is a serious complication that requires lengthy and expert management. Changing access site when indicated may lessen additive effects that contribute to progress of lymphedema.