Knowledge, Confidence in Utilization, and Factors Associated with Integration of Genetics and Genomics into Oncology Nursing Practice
- 1. Department of Nursing Science, University of Ibadan, Nigeria
- 2. Department of Nursing Science, University of Ilorin, Nigeria
ABSTRACT
Purpose: Personalized nursing is becoming the order of the day, hence nurses need to be prepared to engage with genetics and genomics in practice, in order to attend to individual patient needs. There is therefore a need to identify factors that could impede integration of genetics and genomics into practice among nurses working in oncology units of a Nigerian Tertiary hospital, with the aim of providing lasting solutions to them before genetics can be integrated into oncology nursing practice.
Design: The descriptive cross-sectional study design, using the in-depth interview was used for the study. The data was recorded, transcribed and grouped into themes and sub themes. Responses to questions were analyzed thematically.
Results: Results from the study show that the greatest proportion of the participants were Bachelor of Nursing Science degree holders and 40.0% had 20-29 years of experience in nursing practice. Responses gotten from assessment of knowledge showed a poor knowledge of genetics and genomics as about 60% of them were not able to associate it with genes and hereditary. Also, about 95% of the participants implicated the following factors: availability of human resources, time, lack of priority for genetics in healthcare and healthcare records, shortage of staff, heavy workload, lack of motivation, financial implications, lack of interest on the part of patients among other factors.
Conclusion: It is important to identify factors that may impede integration of genetics and genomics into oncology nursing practice, as a way to improve nurses’ readiness for its use in practice.
KEYWORDS
- Nurses
- Integration
- Knowledge
- Genetics and genomics
- Factors Oncology nursing
CITATION
Ani OB, Adejumo PO, Ojo AI, Aluko JO, Ojewale LY (2021) Knowledge, Confidence in Utilization, and Factors Associated with Integration of Genetics and Genomics into Oncology Nursing Practice. Ann Nurs Pract 8(1): 1121.
INTRODUCTION
The terms genetics and genomics are frequently used interchangeably in literature; however, they are distinct terms. Genetics is perhaps the more familiar term; however, genomics has a “broader and more ambitious reach” The National Institute of Health (NIH), [1] defines genetics as the “study of genes and their roles in inheritance of disease,” while genomics involves “the study of all of a person’s genes, including the interaction of genes with each other and with the environment”.
Of increasing importance in all spectrum of healthcare, including health promotion, disease prevention, screening, diagnosis and treatment of diseases, is the integration of genetics and genomics into patient care. However, most oncology nurses have received little or no formal education on integrating genetic and genomic characteristics into patient care. In order to remain integral members of the health-care team, nurses must begin to incorporate genomics into their research and to translate genomic findings into clinical practice. It can therefore be argued that genomics has major implications for the entire nursing profession regardless of their academic preparation, role, or practice setting [2].
More so, Nurses in Nigeria need to be at par with advancements in the field of genetics as are their colleagues from other parts of the world, who seem prepared to engage with genetics and genomics in practice, in order to prevent many undiagnosed and missed cases of cancer, and to reduce death rate from cancers. This provides an underpinning for a study knowledge and factors affecting integration of genetics into practice among nurses working in oncology units.
MATERIALS AND METHODS
This study was based on qualitative data from 15 in-depth interviews that were conducted at University College Hospital (UCH; Ibadan, Nigeria) between February 1st to February 12th, 2020. Qualitative data were collected using in-depth interviews from 15 Nurses working in oncology units of the hospital. A convenience sampling technique was used to select nurses working in the different oncology units of UCH-radiotherapy clinic, radiotherapy ward, nuclear medicine department, as well as West 2, West 3, Southwest 2, FDM, Southeast 2, west 1 and East 1. Nurses working in selected units were approached by the researcher and informed consent were collected from them. In total, 15 consenting nurses participated in the study Some demographic characteristics were obtained from participants.
Participants were asked questions about their knowledge about genetics and genomics, confidence in utilizing genetics and genomics in practice, factors affecting utilization of genetics in practice, effects of social system on integration of genetics and genomics into practice and how best genetics and genomics can be integrated into practice. All questions were open ended and asked in a way that allowed patients and relatives to elaborate on topics that were seen as most important to them. Responses were recorded verbatim and transcribed manually.
This study was part of a larger study, titled “Nurses’ Preparedness for Integrating Genetics and Genomics into oncology nursing practice in a tertiary hospital in Nigeria” Ethical review committees of UCH/UI approved the larger study.
ETHICAL CONSIDERATIONS
Approval for the study was sought from the UI/UCH Ethical Review Committee and attached to the project. Informed consent was obtained from the respondents after explaining the research purpose.
RESULTS AND DISCUSSION
Results from the study show that all the participants were females. The greatest proportion of them, 60.0% were Bachelor of Nursing Science degree holders, 53.3% were Chief Nursing Officers and the greatest proportion, 40.0% had 20-29 years of experience in nursing practice. Responses were presented according to objectives addressed.
Responses gotten from assessment of knowledge showed a poor knowledge of genetics and genomics as about 60% of them were not able to associate it with genes and hereditary. This is reflected in the response below:
Genetics? Is it not about eehmm…(Pauses) Genetics? It has to do with eeehm… I think it is important in various fields like medicine, engineering and others. I can’t really say much
about it but those are the few things I know
I don’t have an idea
A good number of the participants first learnt about genetics in school. Some responses are stated in the figure
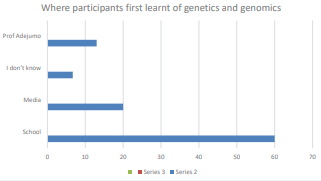
Figure 1 Where participants first learnt of genetics and genomics.
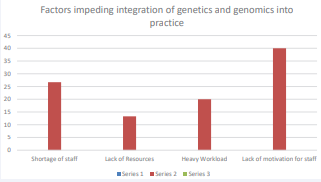
Figure 2 Factors Impeding integration of genetics and genomics into oncology nursing practice.
Relating to perceived importance of genetics and genomics in oncology practice, most of the participants agreed that genetics and genomics is important in order to identify individuals at risk of developing a disease. Some of the responses included:
I think it’s important because, at this level we’ve understood that some or most of these oncology conditions are hereditary. So, we need to educate or kind of counsel our patients for them to understand it more, in order to be able to reduce the rate of occurrence in their family
Hmmmm… You know that we don’t really know the cause of cancer but we know that some are inherited. If a mother has breast cancer the offspring too can have it. It is important we study it so that we know how to prevent and early treatment for people whose parents have cancer
Nurses were further asked how confident they were in integrating genetics and genomics into practice. Approximately 92% of them have never utilized genetic and genomics in practice. Some however stated they utilize genetic terms in passing, making statements such as:
Nooo, no no no. It’s only that when we are admitting patients in our nursing process that we ask questions to find out if the actual disease condition has occurred in the family before. Usually we ask if it has happened to the mother or the father or the siblings or immediate cousins
Participants were asked whether there were rules about how to utilize genetics and genomics in practice. About 80% of them stated there are no rules, but sporadic inclusion in nursing care. The following statements support such:
There are but not really a laid down rule. It is part of the things we learn from the job and even while in school to be able to come down to the level of the patient. It’s like a teacher. Being able to come down to their level and being able to get really deep and ask them questions.
Not much. The only aspect that we practice is during history taking. We want to find out the family history and then if they have young ones that can still be counselled, we refer them to public health nurses for proper counselling. To prevent the occurrence in children and further spread in the family
Participants were further probed on effects of social system on integration of genetics and genomics into practice, and they were asked who the possible influencers in integrating genetics and genomics into practice are. About 97% of the participants identified health care workers as the possible influencers in integrating genetics and genomics into practice, with some of them stating that:
I think nurses are number one because we are at the center of care. We always are in contact with our patients 24/7. If we are given the knowledge, we should be the right people to give this genetic counselling
All health workers can influence. Starting from the Doctors, Nurses, in fact, all health workers
We, the health workers
Participants were further probed on policies they expect the hospital administration to institute to enable them utilize genetics and genomics in practice. About 95% of the nurses stated that training and creating awareness must be key with the following statements:
There should be a department for it. That’s number one. They should create awareness amongst the health workers first before spreading to the general public
Policies……there should be general workshops and seminars. Creating awareness about genetics and genomics, the importance and what it is all about by healthcare workers. During the time of HIV workshops were done. If all these things are done, we can always incorporate into our health routine practice
Participants were further asked what can affect their utilization of genetic and genomic concepts in practice. Factors recognized by approximately 90% of the nurses include knowledge of nurses and shortage of staff.
Some other responses include:
Hmmmm… Time issue can affect it ohh because we are very busy in UCH but I believe there’s a person in charge now. Anyway’ another thing is staff. If we have enough hands, then the people in charge will be able to utilize it well.
It is time consuming. For instance, in a shift we have about 4 to 5 patients in admission and you have to take all those family histories and we are not much. We are short staffed and when it’s like this, you’d be unable to take proper history because you are time conscious. You tend to be in a hurry. So, I think those are part of the disadvantages. It’s time consuming. Then, the willingness of the patient to open up.
Participants were asked whether the atmosphere of their workplace permits integration of genetics and genomics into practice. A good number of the participants, about 70% stated that the atmosphere of the workplace does not permit integration of genetics and genomics into practice with the following statements
Ah! This UCH? No!
Hmmmm…(pauses) not fully because as you can see there’s no privacy. We don’t have enough rooms. We need privacy for counselling because sometimes when you are asking them questions some will cry and some will be moody and you know all these people, sometimes they’ll even throw tantrums even to Nurses.
Well, (pauses) sincerely, no because the work is too much but like you know Nurses can adapt to any situation. If it something that is a laid down rule or something that is laid down, we’ll know how to manage ourselves and attend to it
Answers promptly Naaaaaa….. No it doesn’t
Nurses were further probed on how best genetics and genomics can be integrated into practice. About 95% of them stated that In-service training, patient education, scholarship to study genetics and genomics in school, short courses on genetics and genomics and change in hospital policy to include genetics in practice. Some of the responses include:
It will be integrated right from student curriculum. So, they already know about it. It should be part of the hospital policy. When it is part of the hospital policy, you know that it is expected of you to do it. It becomes a norm. It is the health worker that’ll educate the patients. If the health workers are educated, they’ll pass on what they know to the patients.
Provision of a particular place for that area where the patients will know that, that is their own shelter and when it is your specialty, you’d be able to do things the way it should be done. So, provision of a place, financial support, gathering people with interest, enlightening health workers about genetics through things like scholarships, short courses and In-service Training.
Well, number one is when you educate Nurses, training them from school, then, make it part of the curriculum. Another way is by making standard operating procedure (SOP) and giving a job description to it so that Nurses will know what to do. Then, we should always assist our Nurses too. So, that will stimulate people to do more.
Table 1: Socio-Demographic characteristics of the respondents (n=15).
| Variables | Frequency | Percentage (%) |
|
Gender |
15 | 100 |
| Professional qualification Diploma Degree Masters |
4 9 2 |
26.6 60.0 13.3 |
| Cadre/designation CNO ACNO SNO NOI NOII |
8 1 1 3 2 |
53.3 6.67 6.67 20.0 13.3 |
| Years of experience 0-9 10-19 20-29 30-39 Total |
3 4 6 2 15 |
20.0 26.6 40.0 13.3 100 |
DISCUSSION
The optimal integration of genetic services into existing healthcare systems is a concern in many parts of the world. This is especially true in developing/ resource-limited countries, where significant barriers exist, often related to lack of tangible resources, technology, and knowledge transfer. Nurses have a tremendous responsibility and opportunity to become informed about the potential benefits and challenges of genomics discoveries for clinical care [3].
The study findings regarding respondents’ low knowledge of genomics as it relates to practice are similar to those of several other studies including that [4,5, 6, 7, 8, 9], who all reported a lower level of genomic knowledge. It is however known that knowledge translation of genomic knowledge for healthcare in Africa has been challenged by the dearth of genomic data from people of recent African origin [10]. Recent initiatives such as the Human, Heredity, and Health in Africa Consortium (H3Africa) [11-14] aim to build capacity for genomics research in Africa, and are challenging the existing norms [15]. It is therefore imperative that nurses utilize these opportunities with the aim of improving their genetics and genomics knowledge in order to competently provide genetic services in the near future.
Also, approximately 92% of the participants have never utilized genetics and genomics in practice and almost all of them stated it will be very difficult to utilize genetics and genomics in practice, reflecting an average confidence level. In a study by [16], a relative number of midwives, had average confidence level as a measure of preparation towards integration of genetics into practice, which supports findings from this study.
On effects of social system on integration of genetics and genomics into practice, most of the participants identified health care workers as the possible influencers in integrating genetics and genomics into practice. This is especially true in this age of personalized nursing, where care is no longer a one size fits all. Also, most of the participants suggested that through adequate knowledge and awareness by the nursing leaders, the hospital administration and other healthcare workers, it will be easier to integrate genetics and genomics into practice.
In relation to factors that can affect utilization of genetics into practice, most of the participants implicated the following as some of the factors limiting preparedness for integration of genetics and genomics into practice: availability of human resources, time, lack of priority for genetics in healthcare and healthcare records, shortage of staff, heavy workload, lack of motivation, lack of resources/financial implications, lack of interest on the part of patients, lack of education and inadequate knowledge about genetics and genomics. This finding is supported by findings from the study of [17], where the following key barriers were recognized to limit preparedness for integration of genomics into practice: (a) Limited ‘basic and applied’ genomic knowledge, (b) public unawareness of the importance of genomics, (c) limited institutional support for genomics as a priority, (d) limited time and resources, and (e) incompatibility between genomics and participant’s religious and ethical beliefs. Also supporting findings from this study is findings from [18,19], where limited resources to sequence and characterize human genomes from African populations, lack of access to next generation technologies and analytical capabilities in Africa and, policies that are silent on genetics and genomics and curricula that are not adequate in teaching genetics/genomics concepts, leading to limited appreciation of the utility of genomic knowledge in healthcare were recognized as factors limiting preparedness for integration of genetics and genomics into practice. In addition, they also recognized that African countries lack the critical mass of experts in genetics, genomics, data science, and bioinformatics required to implement country-specific genomic nursing driven healthcare. Therefore, cost-effective strategies are urgently required to promote nurses’ preparedness to incorporate genetics and genomics into practice in Africa for quality health outcomes. These barriers therefore need to be adequately addressed in order to aid nurses’ preparedness to integrate genetics and genomics into practice in Nigeria.
This study was limited to a small number of nurses at one tertiary hospital in Ibadan, Nigeria, which may limit the generalizability of its findings to other locations in Nigeria. Many nurses were busy with work and some of them felt that being interviewed was a waste of time; however, by conducting in-depth interviews, we were able to solicit more complete information and views from participants.
CONCLUSION
Genetics and genomics promise to fulfill the need to predict diseases before they occur. It is therefore imperative that Nurses are prepared to utilize such concepts in practice, as patient care is tending towards personalized ones.
ACKNOWLEDGEMENTS
The authors wish to acknowledge the respondents who participated in the in-depth interviews.








































































































































