Respiratory Failure Secondary to Long-Standing Diaphragmatic Hernia Corrected with Noninvasive Ventilation
- 1. Department of Pneumology, Ramony Cajal Hospital, Spain
Absract
A diaphragmatic hernia is a defect in the diaphragm that allows the passage of the abdominal contents into the chest cavity. This pathological entity produces alterations in ventilatory mechanics, leading to respiratory failure, decreased lung volumes and impaired ventilation-perfusion ratio. We report a 63-year-old man with a history of hydatid cyst located at the left diaphragm operated 30 years ago, who presented acute respiratory failure and severe respiratory acidosis and hypercapnic encephalopathy in the context of a restrictive ventilatory disorder secondary to a diaphragmatic hernia. Noninvasive ventilation (NIV) treatment was effective, with correction of acidosis and disappearance of encephalopathic syndrome. The NIV is an essential treatment in these patients prior to surgery, in order to optimize lung function preoperatively, and a fundamental treatment in patients in whom surgical option is not considered.
Keywords
Diaphragmatic hernia, Respiratory acidosis, Noninvasive ventilation
Citation
Mirambeaux Villalona RM, Barreto DB, Alises SM, Díaz-Lobato S (2015) Respiratory Failure Secondary to Long-Standing Diaphragmatic Hernia Corrected with Noninvasive Ventilation. Ann Nurs Pract 2(3): 1031.
INTRODUCTION
The diaphragm is the primary muscle of ventilation. Its function may be impaired in several situations like paralysis, hernias, eventrations and tumors. Diaphragmatic hernias can be divided into two categories: congenital and acquired. From a functionalist perspective diaphragmatic hernia causes a restrictive ventilatory defect increasing the pressure in the affected hemithorax and compressing the lung parenchyma, favoring the appearance of pulmonary atelectasis. The detection of this entity is a real challenge since most are asymptomatic. Although it can get complicated producing acute respiratory failure, severe respiratory effort with use of accessory muscles, blood gas alterations, decreased level of consciousness and or gastrointestinal complaints. Noninvasive ventilation (NIV) is a useful tool for the treatment of complications of diaphragmatic hernias, as it improves alveolar recruitment of the affected area, while simultaneously increasing the functional residual capacity and minute volume, which leads to better oxygenation tissue. We report a patient with long-standing diaphragmatic hernia who developed respiratory acidosis in the context of severe acute respiratory failure successfully corrected with noninvasive ventilation (NIV).
CASE REPORT
A 63 year-old and nonsmoker man with medical history of left diaphragmatic hydatid disease treated by surgical resection for 30 years. Patient was admitted to the emergency department with progressive dyspnea on minimal effort and daytime sleepiness which started thirty days prior to admission. Physical examination revealed tachypnea (25 breaths per minute), mild subcostal retractions, oxygen saturation by pulse-oximetry (SpO2) 76%, and decreased level of consciousness (Glasgow scale 13/15). Decreased breath sounds at the left lung field on auscultation. The blood test showed 12,200 leukocytes/ml (95.1 percent neutrophils, 4.3 percent lymphocytes), hemoglobin 15.2 grams per deciliter (g/dL). There was severe respiratory failure on arterial blood gas analysis (pH: 7.17; partial pressures of carbon dioxide [pCO2 ] 100 mmHg; partial pressures of arterial oxygen [pO2 ] 58 mmHg; bicarbonate concentration [HCO3 ] 36 mmol /liter; arterial oxygen saturation [SaO2 ] 81%). Chest x ray revealed left basal atelectasis, air-fluid levels, ipsilateral hemidiaphragm elevation with irregular edges and mediastinal shift to the contralateral side (Figure 1).
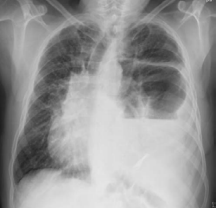
Figure 1 Left basal atelectasis, air-fluid levels, ipsilateral hemidiaphragm elevation with irregular edges and mediastinal shift to the contralateral side.
Noninvasive mechanical ventilation (NIV) was established with bilevel pressure (Stellar® 100, ResMed) with a face mask. Initial settings were inspiratory positive airway pressure (IPAP) of 16 cm H2 O and expiratory positive airway pressure (EPAP) of 6 cm H2 O and oxygen added to 10 liters per minute (lpm). Within an hour of starting NIV there was marked improvement in respiratory rate, which fell from 25 to 19 breaths per minute. Also dyspnea decreased and a significant improvement in blood gases was noted, but sleepiness persisted. Arterial blood gases showed persistence of respiratory acidosis. After 12 hours of NIV, the patient demonstrated significant clinical improvement in the work of breathing, level of consciousness, and arterial blood gas results with complete resolution of respiratory acidosis. Computed tomography (CT) showed a large left diaphragmatic hernia with secondary herniation of almost all of the stomach, splenic flexure and most of the transverse colon, with a voluminous hernia affecting posterior two thirds of the left hemidiaphragm (Figure 2).

Figure 2 Voluminous left diaphragmatic hernia with secondary herniation of stomach, splenic flexure and most of the transverse colon.
Spirometry revealed a moderate restrictive ventilatory pattern and normal diffusion test. Polysomnography showed severe obstructive sleep apnea syndrome with time oxygen saturation <90% (T90) 75% and respiratory disturbance index (RDI) 59.4. Arterial blood gases showed chronic hypercapnic failure (pH: 7.36; PCO2 : 55 mmHg; PO2 : 50 mmHg; HCO3 : 31 36 mmol /liter; SaO2 : 83%). Nocturnal home noninvasive ventilation was indicated. Six month later, the patient was asymptomatic and had arterial blood gases into normal values.
DISCUSSION
A wide variety of restrictive thoracic diseases have been successfully treated with NIV, including thoracic cage abnormalities (eg, chest wall deformities, kyphoscoliosis, spinal cord injury, and sequelae of polio), in addition to both rapidly and slowly progressive neuromuscular conditions (eg, amyotrophic lateral sclerosis [ALS] and a medley of myopathic/neuropathic disorders) [1,4].
The mechanisms by which NIV treatment exerts a positive impact on both day and nighttime symptoms and gas exchange remain unclear, but several basic theories exist and are likely complementary rather than contradictory. The three basic proposals include the following: (1) respiratory muscle rest; (2) resetting the CO2 sensitivity of the central ventilatory controller; and (3) changes in pulmonary mechanics [1].
The improvement in daytime spontaneous arterial blood gas values alone has been offered as testimony to resetting of the centrally determined CO2 set point, but others have definitively shown augmentation of both hypoxic and hypercapnic ventilatory responses in a patient with central apnea treated with NIV. The positive response may be mediated, in part, through changes in sleep fragmentation, the depression of arousal mechanisms, and alterations of sleep architecture. Lastly, NIV may raise lung volume, improve lung compliance, and reduce dead space by recruitment of atelectatic lung associated with respiratory muscle weakness [1].
We present the case of a patient with an acute respiratory failure, severe respiratory acidosis and hypercapnic encephalopathy secondary to a restrictive ventilatory defect produced by an acquired diaphragmatic hernia. The patient was treated with NIV and showed clinical improvement. Patient was discharged home with noninvasive ventilation and showed a good clinical evolution
Diaphragmatic hernias are defined as the passage of abdominal contents into the thoracic cavity through a diaphragmatic anatomical defect. They are classified as congenital (anterior or Morgani’s), posterolateral (or Bochadalek’s), and acquired (traumatic) [2,3]. Congenital diaphragmatic hernias produce pulmonary hypoplasia and pulmonary hypertension in the newborn, which are associated with life-threatening physiologic complications. Traumatic diaphragmatic hernias result from blunt or penetrating trauma.3 Most of hernias are small defects caused by the pressure difference between the abdominal and chest cavity. The thorax is occupied by a voluminous hernia that causes a severe restrictive ventilatory defect. The pathophysiology of traumatic diaphragmatic hernia includes both respiratory depression and circulatory secondary to decreased diaphragmatic excursion, lung compression by the herniated contents, increasing the pressure in the affected hemithorax and mediastinal shift to the contralateral side.3
A diaphragmatic hernia has indication for surgical correction depending on if the injury is acute or chronic [3]. If the diaphragmatic injury is discovered during the acute phase of trauma, the standard surgical approach is laparotomy or, less commonly, thoracotomy. The problem regarding which approach to use arises when the diaphragmatic injury goes unnoticed for months or years. More surgeons approach long-standing hernias via a transthoracic or thoracoabdominal approach because the herniated intra-abdominal contents tend to be firmly attached to intrathoracic structures, making a transabdominal approach difficult [5].
In our case surgery was not performed because of the surgical high-risk. In patients with complicated diaphragmatic hernia mortality risk increased by 5.3% [6]. Therefore, we used NIV as the first-line treatment for acute respiratory failure [7]. NIV is an essential therapy to optimize lung function preoperatively, and it is an important alternative treatment in patients in whom surgery is not indicated.8
8Increasing positive end expiratory pressure (PEEP) to 15 cm of H2O does not affect the intra- abdominal pressure (IAP). This was confirmed by Guimaraes and animal data. However, on increasing PEEP to 15 cm of H2O, some researchers have found only a mild increase in IAP in patients with a baseline IAP below 12 mmHg [9]. Moreover, PEEP matched to intra-abdominal pressure led to increased lung volumes and oxygenation and decreased chest wall elastance shunt and dead-space fraction [10]. Clinical studies trials had sown the feasibility and clinically efficacy of NIV applied in selected patients with acute respiratory failure including after abdominal surgery. It´s also recommend as an alternative to conventional ventilation in selected patients with acute respiratory failure after abdominal surgery who require ventilatory support [11,12]







































































































































