Tibial Pilon Fractures
- 1. Department of Orthopedics, Hospital of Avila-sacyl, Spain
- 2. Department of Orthopedics, Hospital Severo Ochoa, Spain
- 3. Department of Orthopedics & Trauma Surgery, University of Valladolid, Spain
- 4. Department of Orthopedics, University of Valladolid, Spain
- 5. Department of Orthopaedics & Trauma Surgery, Marqués de Valdecilla University Hospital, Spain
- 6. Department of Orthopedics Surgery and Traumatology, Hospital of Ávila, Spain
Citation
Martín OF, Acosta PZ, Castrillo AV, Martín Ferrero MÁ, De la Red Gallego MÁ, et al. (2016) Tibial Pilon Fractures. JSM Foot Ankle 1(1): 1001
INTRODUCTION
Tibial pilon fracture was described by the French radiologist Etienne Destot [1,2] in 1911. This fracture (1- 5 % of lower limb and 7 - 10% of all tibial fractures) [3] is intra-articular extending into the tibiotalar joint and might be the result of high or low energy traumatism [3-5]. The main lesion mechanism is due to axial compression of the talus into distal tibia that may associate rotational forces depending on the injury direction and foot position [3,4].
There groups of pilon fractures are described depending on pathophysiology [2]: group A associates high energy injury with important soft tissue affection, comminution and impaction; group B includes rotation injuries and it does not usually present cartilage impaction; group C are fractures in elderly patients, typically with osteopenia and due to low energy trauma [6-8].
Diagnosis of the fracture is given by clinical examination and determined by images complementary testing of the ankle. Treatment strategy in fact will be determined by fracture lines, tibiofibular lesions associated, comminution and depression of the articular surface [9,10]. The associated soft tissue injury can be the most concerning and often has a significant influence on the overall treatment strategy and results [9-10].
CLASSIFICATION
Standard ankle radiographs and full-length radiographs of the tibia and fibula are required to identify fracture extension [11]. CT is useful to determine the articular involvement and preoperatively to add information about the best surgical approach. AO foundation and orthopaedic trauma Association (AO/OTA) and Ruedi and Allgower are the two main classifications. Ruedi and Allgower [12] described pilon fractures in three types: I) non-displaced intraarticular fractures; II) displaced fractures with loss of articular congruency; III) severely comminuted fractures with impaction of the distal tibia
In the AO classification [13] pilon fractures are classified as 4.3. The first number indicates tibial location and the second one represents the segment bone. Then letter A is used for extraarticular fractures, B for partial articular fractures and C means complete articular injury without continuity between diaphysis and the articular segment.
Topliss [5] reviewed 126 fractures and by means of CT evaluation divided fracture pattern in sagittal or coronal, based on the main fracture line. Sagittal fractures are associated to high energy injury with varus angulation meanwhile coronal fractures are related to less severe injury in elderly people with valgus angulation of the ankle.
Tang [14] proposed a four column classification evaluating anatomical fracture pattern by a CT and also associating a clinical decision making. Due to anatomical pattern location such as anterior column, posterior column, medial column or lateral column, they recommend a posterolateral approach, anterior, medial or posteromedial approach respectively.
TREATMENT OPTIONS
Conservative treatment could be used in non-displaced fractures, non-walking patients or severe pluripathological diseases [13]. However this kind of treatment is exceptionally indicated. Ruedi and Allgower [14] presented good results with open reduction and internal fixation (ORIF). They created classic principles of treatment based on plating the fibula to gain length, articular reduction and reconstruction, bone grafting of tibial metaphyseal defects and providing a medial buttress with an internal plate. These authors had good results with early ORIF but coronal fractures described by Topliss [5] and fractures with anterior comminution presented failure of the osteosynthesis due to an insufficient stabilization with a medial plate.
ORIF technique can be elected in one or two stages. There are different schools with good results in early intervention with a single stage [14,15] but nowadays, majority of surgeons defends and ORIF in two stages [16-18] due to the cutaneous complications. Vascularity of the overlying skin will recover in most cases after 10 to 14 days of the initial trauma.
ORIF in two stages consists on temporary stabilization with an external fixation in the first stage and followed by a definitive internal fixation [19,20]. Definitive fixation takes places usually two weeks after the external fixation when skin is in adequate conditions. It can be checked by the wrinkle sign as it demonstrates resolution of swelling and edema.
The advantages of two stages are the optimum management of soft tissue and the ability to maintain anatomic realignment of articular surface under direct visualization. However, joint reduction with external fixation often is insufficient, secondary stiffening of the ankle and usually infection of the pin tract may occur [20]. Medial internal osteosynthesis in two phases presented 2-10% of infection, 0-8% bad reductions and 2-5% of mal unions [2].
Initial fibula fixation remains controversial. Fibular osteosynthesis is recommended because restores length and rotation. However it is necessary to take into account that this fixation might compromise a future antero-lateral approach to the tibia (7 cm bridge skin is recommended between incisions), that tension applied to the skin might be increased and that it would not allow the option of shortening tibia in type C fractures [21].
Approach must be chosen depending on the main line of fracture [13]. Anterior approach, medial to the tibial anterior tendon, provides good exposure. Posteromedial complementary approach is sometimes needed to allow reduction and fixation of posterior fragments [22]. Exclusive posteromedial approach is not usually recommended due to complications and bad reductions [23].
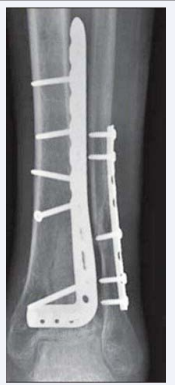
Locking plate fixation is a good option to choose in patients with osteopenia or comminution due to its better stability (Figure 1).
Figure 1: Locking plating for tibial pilon fracture and fibula stabilization
However its thickness may not reduce cutaneous complications [24] and its great stability sometimes lead to bone union delay [25].
Percutaneous synthesis through minimal approaches (MIPO) has been described [2]. This technique preserves osseous vascularity and fracture hematoma which provides a better biological repair but it has contraindications such as cutaneous lesions and central subsidence of the joint.
Siddhartha [26] presented 50 cases of MIPO locking plate fixation with a mean fracture healing of 21.4 weeks, 10% superficial infection and deep infection, implant failure and malunion in 2% cases. Borens [27] used a two stage MIPO series with non-locking low profile plate and also reporting good results.
Definitive external fixation is another kind of treatment for pilon fractures. The principle is to reestablish alignment, stabilization of the fracture and restoration of the joint surface [2].
External fixation as a definitive treatment is a good technique for some type C injuries. The different constructs of external fixation are simple bridging frames, ankle distraction and hybrid or circular frames used in conjunction with limited internal fixation of the joint by minimal incisions or percutaneous [28- 32].
Endres [33] showed advantages of hybrid external fixation for comminuted type C fractures. In its series there were no deep infections, no secondary arthrodesis and 87% of the cases had good functional results. No differences have been described in bone union time between circular external fixation [34] and hybrid external fixation [35] comparing with ORIF. A meta-analysis by Wang [36] showed no difference in bone healing between ORIF and external fixation with limited osteosynthesis. It also demonstrated no difference in non-union, delay union or superficial or deep infection.
Watson [37] demonstrated good results of bone union and less skin complications with circular external fixation in patients of severe contusion or opens fracture comparing. Deep infections are prevented with daily cleaning pin care, without applying fixation on cutaneous tension and removing wires with surgical debridement when inflammatory signs are presented [2].
Arthrodesis is another surgical treatment for lesions with severe comminution [38]. Primary ankle arthrodesis restores acceptable function and reduce period of disability and severity of sequelae [38,39].
In relation to bone defects, autologous bone grafting is used in small ones. Vascularized fibula segment decrease time of bone healing and demonstrated better resistance to infection [40]. Masquelet technique is an option of bone grafting but it needs two surgeries to be realized [41]. Tibia could be shorted and it may be a good technique when injuries of soft tissues or comminution are present [42]. In cases of larger bone defects bone transport is an option but it has higher complications rates [43-46]. Arthroscopy is a method not widely used in the treatment of these fractures [47,48]. Treatment of open fractures needs debridement and skin cover, stabilization and bone grafting if bone loss is presented [49]. Vacuum assisted closure (VAC) could be used to cover large wounds temporally. Definitive flap cover closure should be done with definitive stabilization [1,2].
COMPLICATIONS
Tibial pilon fractures present several complications such as secondary displacement, cutaneous necrosis, infection and arthritis [49]. Cutaneous necrosis is a frequent complication in high injury fractures. Surgical cleaning, antibiotics and VAC treatment is a good option but tenuous vascularity usually requires plastic surgery to cover it.
Infection complication should be treated with curettage, antibiotics and sometimes removal of the material used. Meticulous management of soft tissue and direct approach of the fracture minimized to 2% the infection rate [49]. Secondary displacement is more often in varus and it is due to insufficient osteosynthesis [5]. Greater than five grades of varus should be corrected by re-reduction and re-synthesis. Arthritis is well tolerated by patients but some cases require arthrodesis.
CONCLUSION
Tibial pilon fractures are intraarticular complex fractures. The treatment objectives are to restore the articular congruency and mechanical alignment to allow early rehabilitation while minimizing soft tissue complications. Surgical treatment is based in skin injury, fracture pattern and surgeons experience. Open fractures need debridement and definitive fixation must be done with soft tissue coverage. Fractures with comminution and high energy trauma are better to treat with a two stages ORIF. When large comminution is presented, arthrodesis and tibia shortening are options to consider. MIPO techniques are marking the surgical tendency in the treatment of these lesions.
REFERENCES
9. Scolaro J, Ahn J. Pilon fractures. Clin Orthop Relat Res. 2011; 469: 621- 623.
16. Sirkin MS. Plating of tibial pilon fractures. Am J Orthop (Belle Mead NJ). 2007; 36: 13-17.
18. Sommer C, Pesantez R. Tibia and fibula distal minimally invasive plate osteosynthesis. 2012; 545-562.
20. Dake T, Fang J, Hao Z, Wenbin D, Yang W, Ping C, et al. Int Orthop. 2012; 36: 833- 837.