A Rare Case of Male Breast Plasmacytoma.
- 1. NKP Salve Institute of Medical Sciences, Maharashtra University of Health Sciences, India
Abstract
A plasmacytoma is a discrete, solitary mass of neoplastic monoclonal plasma cells in either bone or soft tissue (extramedullary). Breast plasmacytomas, in particular, are extremely rare and can present as a primary isolated tumor or as an extramedullary manifestation of multiple myeloma (MM). Microscopically, immature plasmacytomas may mimic other neoplasms, so caution should be made on histological examination to ensure the correct diagnosis and corresponding therapy. We present a case of 57 year old male, who was a known case of multiple myeloma and on regular medication for the same, presented with complaints of swelling of right breast. Excision of the lump was done and histopathological examination was suggestive of plasmacytoma.
Keywords
• Multiple myeloma
• Breast plasmacytoma
• Male breast plasmacytoma
• Extramedullary plasmacytoma
Citation
Gedam BS, Soni N, Sadriwala QS, Kale VB, Bansod PY (2017) A Rare Case of Male Breast Plasmacytoma. JSM Gen Surg Cases Images 2(4): 1039.
INTRODUCTION
A plasmacytoma is a discrete, solitary mass of neoplastic monoclonal plasma cells in either bone or soft tissue (extramedullary) [1]. There are three entities of plasmacytoma: solitary plasmacytoma of bone, extramedullary plasmacytoma, and multiple solitary plasmacytomas that are either primary or recurrent.
Breast plasmacytomas, in particular, are extremely rare and can present as a primary isolated tumor or as an extramedullary manifestation of multiple myeloma. Microscopically, immature plasmacytomas may mimic other neoplasms, so caution should be made on histological examination to ensure the correct diagnosis and corresponding therapy. Plasmacytoma of the breast, either as a solitary extramedullary plasmacytoma (SEP), or as evidence of dissemination of Multiple Myeloma (MM), is exceedingly rare. Only 63 cases were reported from 1928 to 2009 [2]. We present a histologically diagnosed case of male breast extramedullary plasmacytoma.
CASE PRESENTATION
A 57 year old gentleman who was referred to us with complaint of swelling in right breast since one month which was gradually increasing in size. There was no history of nipple discharge, skin retraction, weight loss or any previous history of trauma.
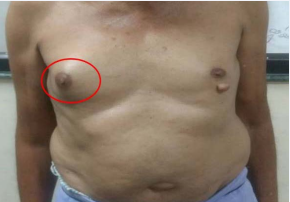
On examination, a lump of 5 x 4 cm was palpable behind right nipple areola complex. Lump was firm, non-tender & not fixed to skin or underlying muscle on palpation. The axillary lymph nodes were not palpable (Figure 1).
Figure 1 Clinical photograph showing 5x4 cm lump in right breast.
Patient was a known case of multiple myeloma since 1 year for which he was on regular medication; Mephalan (5mg), Dexamethasone (4mg), Thalidomide (100mg), Calcium and Vitamin D3 supplements, Bisphosphonates (Zolendronic acid 1mg). Histology of bone marrow aspirate was suggestive of bony fragments with plasma cells suggestive of plasma cell dyscrasias. Bence Jones proteins were negative in urine.
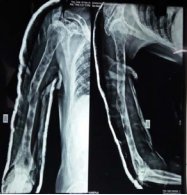
Patient also had a history of pathological fracture of right humerus one year back, which was managed conservatively. Also, previous x-rays showed lytic lesions of pelvis, sacrum and lumbar vertebral bodies; diffuse osteopenia; decreased intervertebral space in T12-L1 and T11-T12. Few lytic lesions noted giving ‘rain drop appearance’ suggestive of metastasis or multiple myeloma (Figure 2-4).
Figure 2 X-ray right humerus showing pathological fracture.
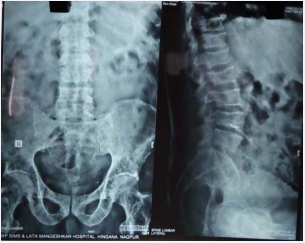
Figure 3 X-raypelvis, sacrum and lumbar vertebral bodies showing lytic lesions; diffuse osteopenia; decreased intervertebral space in T12-L1 and T11-T12.
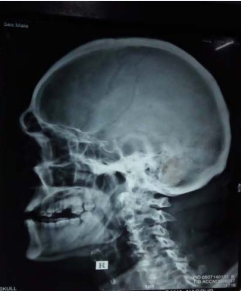
Figure 4 X-ray skull showing few lytic lesions giving ‘rain drop appearance’.
Sonomammography of right breast was suggestive of mass lesion noted in right breast in retro-areolar region, appeared to be solid mass with heterogeneous echotexture with few lobulations.
It measured 4.5 x 3.9 x 3.4cm. Mild vascularity noted on colour doppler. Mass was extending up to the muscle plane. No axillary lymphadenopathy.
Fine needle aspiration cytology (FNAC) of the lump was suggestive of lymphoproliferative disease/plasma cell disease.
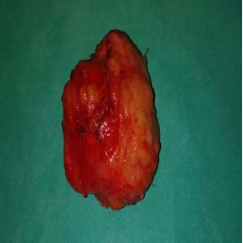
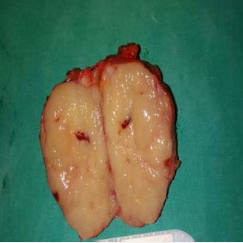
Patient underwent excision of the lump. Transverse incision given over the swelling on right side. A well circumscribed, partly encapsulated greyish white mass of size 5 x 3.5 x 3cm was noted. Mass was excised. On cut-section, a homogenous white surface was noted (Figure 5, 6).
Figure 5 Excised mass showing a well circumscribed, partly encapsulated greyish white mass of size 5 x 3.5 x 3 cm.
Figure 6 On cut-section: Homogenous white surface noted.
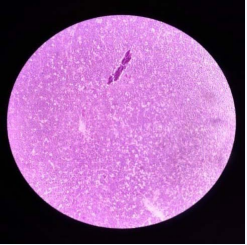
On histopathological examination, sheets of moderately sized monomorphic population of cells with round to oval vesicular nuclei with clumped chromatin. Mild to moderate anisonucleosis. Sheets of tumour cells mostly scattered singly with high NC ratio and focal plasmacytoid change. Features were suggestive of plasmacytoma (myeloma deposits) (Figure 7).
Figure 7 Histopathological examination.
DISCUSSION
Plasmacytoma, a neoplastic proliferation of plasma cells, is one form of plasma cell dyscrasia. Plasmacytoma may be primary or secondary to disseminated multiple myeloma and may arise from osseous (medullary) or non-osseous (extramedullary) sites. [1] Solitary Bone Plasmacytoma (SBP) represents plasma cell dyscrasia with a single bone involvement (localized form) due to a malignant plasma cell infiltrate [3]. The most common sites of SBP are long bones and vertebrae. [3] In a review of more than 400 published articles, 82.2% of extramedullary plasmacytomas were found in the upper aerodigestive tract with 17.8% arising in the gastrointestinal tract, urogenital tract, skin, lung, and breast in that order. [4]
Plasmacytoma of the breast, either as a solitary extramedullary plasmacytoma (SEP), or as evidence of dissemination of Multiple Myeloma (MM), is exceedingly rare. Only 63 cases were reported from 1928 to 2009 [2].
Most (75%) plasmacytomas of the breast occur during relapse of MM. Most breast plasmacytomas occur in women with a mean age of 53 years at diagnosis, but predominantly unilateral. Databases screened from 1988 to 2009, retrieved a total of 9 male patients with breast plasmacytoma [5]. Since 2009, no case of male breast plasmacytoma was reported in the literature.
Both primary and secondary plasmacytomas can be misdiagnosed as primary breast carcinoma or even a benign disease [3]. FNAC or trucut biopsy has proven to be an excellent method in diagnosing primary and secondary malignancies [6]. Plasma cells can be separated from other white cells based on strong CD38 and CD138 expression [7-9].
Expression of CD56 is commonly used to identify abnormal plasma cells, since normal plasma cells are typically CD56 negative. CD56 expression has been associated with poor outcome in myeloma patients. The initial treatment for a myeloma patient would depend upon whether or not the patient is a candidate for stem cell transplantation [7,10-13].
In eligible patients, high-dose chemotherapy with autologous stem cell transplantation (ASCT) has become the preferred treatment for patients under 65 years of age [14,15]. Adjuvant chemotherapy should be considered in patients with tumours greater than 5 cm and those with high grade tumours. Chemotherapy is indicated for patients with refractory and / or relapsed disease [16].
Novel agents like thalidomide, lenalidomide and bortezomib produces a remission in more than 70% cases. Thalidomide has been used to treat SEP in the context of relapsed MM with variable results [14].
In the last 5 years, several new drugs have been introduced into clinical practice greatly expanding treatment options for myeloma relapse patients. These include carfilzomib, pomalidomide, panobinostat, elotuzumab, daratumumab and ixazomib [17].
Solitary plasmacytomas have a good prognosis (radiotherapy and surgery are curative treatment options) and less than 30% of cases develop MM or other plasmacytomas, whereas the disease progresses with unfavorable outcomes in patients with MM and extramedullary plasmacytomas [18].
Plasmacytomas are radiosensitive, with success rates of 79%–90% and a 10-year survival rate of 50%–100% [19].