Atypical Clinical Presentation of Ocular Tuberculosis in an Immunocompetent Patient
- 1. Department of Infectious Diseases, Fattouma Bourguiba Teaching Hospital, Tunisia
Abstract
Background: Tuberculosis (TB) is on the major systemic disease causing mortality and morbidity all over the world. TB may affect any ocular or orbital tissue. The clinical manifestations are not specific and ocular TB may cause severe visual loss in the absence of early and appropriate treatment.
Findings: Here we report a case of a healthy 48-year-old-man presenting with acute lymphocytic meningitis and admitted initially for clinical monitoring. He was noted to have a sudden blurred vision and fundus examination showed Choroid lesion diagnosed as ocular TB. He received full anti-TB treatment but he died within the tenth day of treatment.
Conclusion: Ocular TB is rare and may be revealed by acute lymphocytic meningitis. It should be suspected in any case of visual disorders in endemic areas.
Keywords
• Ocular tuberculosis
• Acute lymphocytic meningitis
• Choroiditis
• Anti-tubercular treatment
Citation
Marrakchi W, Aouam A, Kooli I, Brahim HB, Loussaief C, et al. (2016) Atypical Clinical Presentation of Ocular Tuberculosis in an Immuno-competent Patient. J Neurol Transl Neurosci 4(1): 1061.
ABBREVIATIONS
TB: Tuberculosis; ATT: Anti-Tubercular Treatment
INTRODUCTION
Tuberculosis is a serious infectious disease that affects about a third of the world population [1,2]. Ocular TB is re-emerging as a major challenge all over the world. This disease can involve any tissue of the eye and the orbit. The commonest manifestation is in the uveal tract and usually presents as a posterior uveitis. But the clinical diagnosis of ocular TB is difficult since clinical signs and symptoms can mimic other conditions. Ocular tuberculosis is rare in immunocompetent persons. We are presenting a very rare case of ocular tuberculosis in a healthy 48-year-old man.
CASE PRESENTATION
A healthy 48-year-old man with past medical history of diabetes mellitus type 2 treated with insulin, presented to the emergency room with a five-day history of headache, sudden high fever, photophobia and sonophobia associated with neck stiffness for about two days. There was no history of any ocular surgery or trauma. On examination, he had fever (39° c), Brudzenski and Kernig signs were positive. Pupils were equal and reactive. Skin sensation, muscle tone and cranial nerves were intact. Deep tendon reflexes were normal and Babinski reflex was absent. Lumbar puncture (LP) was done. The cerebro-spinal fluid was clear and contained 900 cells/ml (95 percent lymphocytes). The protein content was 1,04 g/l with a low grade-glucose level equal to 3,5 mmol/l. The chloride content of the fluid was normal. Microbiologic direct exam was negative and revealed the absence of bacilli. Culture was negative. Blood chemistry was unremarkable except for haemoglobin of 10 g/dl. Renal and liver function tests were normal. C-reactive protein was negative. Acute lymphocytic meningitis was initially suspected and the patient was kept under surveillance. Two days after, the patient was noted to have blurred vision and worsening headache. Ocular examination of the two eyes revealed VA 5/10 and bilateral altered pupil reflex. Fundus examination showed multiple big nodular lesions that were bilateral and the presence of perivascular choroidal lesion. It showed also papilloedema which could be associated with optic neuritis (Figure 1).
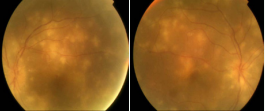
Figure 1 Bilateral multiple big nodular lesions that were bilateral and the presence of perivascular choroidal lesion. It showed also papilloedema.
Tuberculosis was the most likely diagnosis. Brain CT did not show any cerebral lesion that may be correlated with TB (Figure 2).
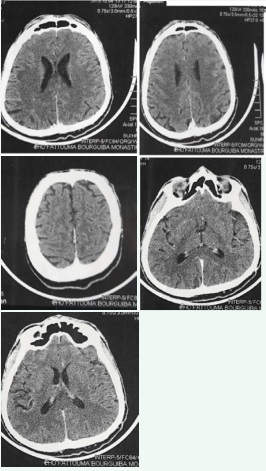
Figure 2 CT scan of brain was normal and did not show any cerebral or optic nerve lesions
MRI brain scan was not done initially. PPD skin testing was positive and the induration was 20 mm. We investigated this patient thoroughly for his immune status including HIV and syphilis screening and were immunocompetent. West Nile virus, Ebstein Barr virus, Cytomegalovirus and Rickettsia antibodies were negative. The diagnosis of presumed tuberculous meningitis associated with tuberculous choroiditis pqpilloedma and optic neuritis was established. After consulting ophthalmologists, we started him on full anti-TB treatment with Isoniazid 300 mg/day, Rifampicin 600 mg/day, Pyrazinamid 1200 mg/day and Ethambutol 1600 mg/day; without systemic steroid because we speculate that cortico-steroids therapy may cause the progression from choroiditis to endophtalmitis. In the tenth day of treatment, the patient was noted to have clinical deterioration with worsening neurological signs, sudden loss of vision and confusion. Fundus examination showed the progression of the chorio-retinal lesion to the macula. The patient presented sudden coma and died before Brain MRI.
DISCUSSION
Tuberculosis is a serious infectious disease caused by acid-fast bacteria belonging to Mycobacterium tuberculosis complex. It affects predominantly the lungs although it can affect every organ of the body [3]. It remains a major global health problem with an estimated 8,6 million people who have developed TB and 1,3 million death in 2012 [2,3]. All parts of the eye may be affected by TB. Tuberculosis is an under-diagnosed etiological agent in the choroiditis, uveitis, and optic neuritis. The most common ocular manifestations are chorio-retinitis and uveitis [3]. The disease affects predominantly young to middle age man. The other factors that may increase the risk of acquiring ocular TB are alcoholism, drug addiction, HIV infection, immunosuppressive conditions and diabetes mellitus. Ocular TB results either from haematogenous seeding from the primary complex or contiguous spread of variable bacilli or as local manifestations of a hypersensitivity reaction to circulating tubercular proteins. Posterior uveitis is the most common clinical presentation of ocular TB, followed by panuveitis, with granulomatous anterior uveitis [4]. The main site is the choroid where the high oxygen tension may promote organism growth. TB-associated choroiditis is usually characterized by multifocal pattern, with chorio-retinal lesions variable in shape, number, size and location [4]. In the present case, the lesions presented as choroidal tubercles which appear as multiple bilateral nodular lesions. Choroidal tubercles are foci of granuloma in the choroid. Nearly 30% of patients with disseminated TB or tuberculous meningitis may exhibit small choroidal lesions [4]. It has been reported in association with meningoencephalitis or meningitis like in our case. According to ophthalmic examination in this case, the optic nerve was also affected and the manifestations were in the form of papilloedema. Optic nerve involvement is a common complication and in our patient, it results from contiguous spread from the choroid. Papilloedema, and in advanced cases, bilateral optic atrophy usually results from central nervous system TB particularly tuberculous meningitis. It is difficult to confirm the diagnosis of ocular TB by laboratory methods. Definitive diagnosis depends on the isolation of mycobacterium tuberculosis from a specimen. The presence of mycobacterium tuberculosis in ocular tissues or fluids should be confirmed either by histology or microbiological investigation. The technique of PCR can detect as few as one organism in the fluids. In our case, clinical examination, fundoscopy, the lymphocytic meningitis and positive PPD skin test led to the diagnosis of tuberculosis. In the absence of definitive evidence, our diagnosis was presumptive. Syphilis, toxoplasmosis, sarcoidosis, brucellosis, histoplasmosis, hemangioma, metastasis, foreign body and amelanotic melanoma are included in the differential diagnosis of ocular TB [5]. The use of anti tuberculosis agents (ATT) to manage presumed ocular TB is regarded as an effective tool for tubercular uveitis and response to therapy can be good surrogate for diagnosis of presumed ocular TB [6]. Standard ATT involving combing therapy with Isoniazid, Rifampicin, Ethambutol and Pyrazinamid is recommended. Treatment is continued for a further nine to twelve month with Isoniazid and Rifampicin [1]. However, there are no agreed upon or standardized guidelines on the length of treatment for ocular TB [1,6]. Steroids for 4-6 weeks concomitant with standard ATT may limit damage to ocular tissues from paradoxical worsening of ocular TB after initiation to ATT. There may be worsening of inflammation following ATT use in patients which may not be controlled with steroids. In such patients immunosuppressants may be added provided HIV and other immunosuppressive conditions are ruled out [3]. This observation suggests that the paradoxical worsening may be due to the oedema in the brain. The dramatic evolution just after ATT is may be caused by allergic reaction to mycobacterium tuberculosis, brain oedema or metabolic disorders.
CONCLUSION
Ocular tuberculosis often poses a diagnostic and management challenge. Detection of choroidal inflammation can prevent visual loss as the ocular lesion resolves fully with timely management [6-9]. This case highlights the fact that suspecting and managing rapidly this condition may improve the visual and the vital prognosis.








































































































































